vaginal wet prep
To see motile trichomonas, here is a link: https://video.search.yahoo.com/video/play;_ylt=A2KIo9dxfr5VflMAx5AsnIlQ;_ylu=X3oDMTByZ2N0cmxpBHNlYwNzcgRzbGsDdmlkBHZ0aWQDBGdwb3MDMg--?p=trichomonas&vid=5a03d4da873f66511d48ac675a396035&turl=http%3A%2F%2Ftse3.mm.bing.net%2Fth%3Fid%3DWN.%252bQDNDyS7XmDMM47nzxtq3w%26pid%3D15.1%26h%3D225%26w%3D300%26c%3D7%26rs%3D1&rurl=https%3A%2F%2Fwww.youtube.com%2Fwatch%3Fv%3D2RKDBd8Dpp0&tit=trichomonas&c=1&h=225&w=300&l=30&sigr=11b1381st&sigt=10bbbsi7p&sigi=12nbf0kkq&age=1196006400&fr2=p%3As%2Cv%3Av&fr=yhs-mozilla-001&hsimp=yhs-001&hspart=mozilla&tt=b
THE WET PREP:
A vaginal wet prep (wet mount or vaginal smear) is a gynecologic test performed as a STAT (within an hour) on a sample of vaginal discharge used to find the cause of vaginosis, vaginitis and vulvitis. Vaginitis symptoms include itching, burning, discomfort, vaginal discharge, odor and/or rash. It assists in the identification of and diagnosis of vaginal yeast infection, trichomoniasis, bacterial vaginosis, and allergic dermatitis. It may also be used in rape investigations to detect the presence of semen.
How to Perform a Wet Prep:
*Add a drop of specimen (if dry, add saline or sterile water) to a clean slide.
*Add a cover slip and read immediately so the slide doesn't dry out
*Look for clue cells, white blood cells, trichomonas, and yeast (cells, budding, pseudohyphae).
*View under the 40x objective lens, turning down the light source to see the hyaline structures. You may add a drop of KOH (potassium hydroxide) and replace the cover slip to look for fungal elements such as pseudohyphae after looking for the other components on the slide, as the KOH will break down other debris, such as bacteria and cells, leaving only fungal elements if there .
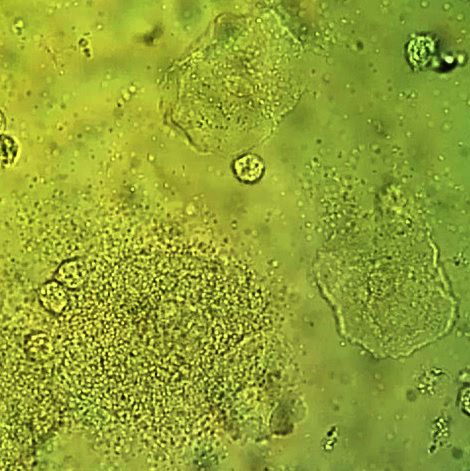
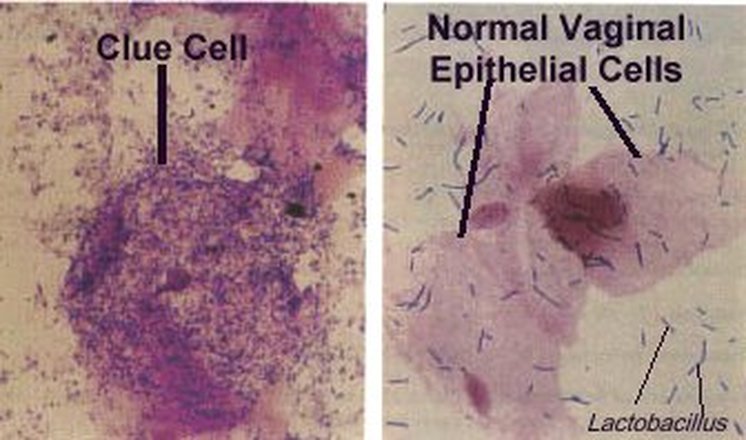
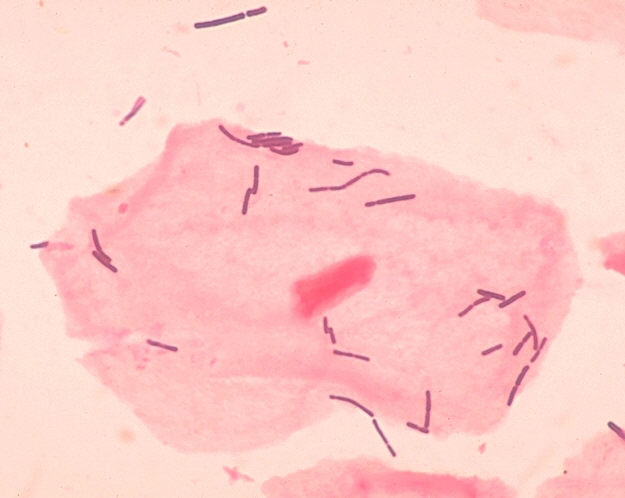
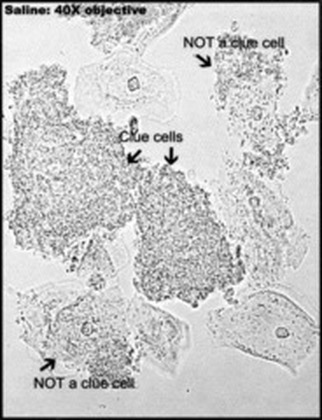
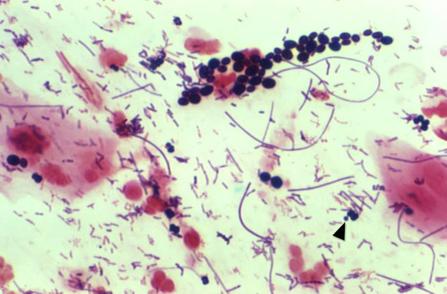
*The image above shows vaginal clue cells covered with bacteria. The edges are no longer visible and the cell looks like sand paper (bottom left). The upper 2 epithelial cells are beginning to be attacked by the mixture of bacteria and you can see the edges beginning to ruffle like a fried egg. Gardnerella vaginalis or Mobiluncus commonly cause the formation of clue cells. Gardnerella vaginalis consists of a mixture of Gram-variable bacteria, such as Gram-positive cocci, Gram-negative coccobacilli, and Gram-negative rods covering the cell. Mobiluncus are curved Gram-negative rods. They may be found along with Gardnerella vaginalis in bacterial vaginosis.
*Lactobacillus (long, slender Gram-positive bacillli/rods) seen on vaginal wet mounts or vaginal Gram-stains is normal, however, and represents good, healthy vaginal flora. You are looking for a mixture of short rods, curved rods, and cocci on the epithelial cells, which cover about 75%-100% of the cell in order for it to be named a "clue cell". When reporting clue cells and bacterial vaginosis, at least 20% of all epithelial cells seen on the slide should be clue cells. A rare clue cell here and there does not truly represent vaginosis. This is in accordance with the CDC standards and Amsel's criterion.
In a normal test, no yeast or Trichomonas will be present on the slide. White blood cells and/or clue cells are usually absent or very low in number. The normal vaginal pH is 3.8-4.5.
Symptoms of Infections Able to be Diagnosed by Wet Mount:
Vaginitis:
Vaginitis is associated with bacterial vaginosis in 40-45% of cases, candidiasis in 20-25% of cases, trichomonas in 15-20% of cases, allergic reactions, dermatitis, herpes simplex virus (HSV), mucopurulent cervicitis, atrophic vulvar vestibulitis, desquamous inflammatory vaginitis, foreign bodies, but is even considered normal in some females.
1) Yeast Infection-thick, white, lumpy, cottage cheese-like discharge; Yeast, buds, and/or pseudohyphae may be present (only seen about half of the time); Other facts:
Amsel's Criteria: a) Discharge is thin/homogenous, b) Sample smells fishy upon the addition of KOH (potassium hydroxide)-"Whiff Test", c) Vaginal pH is >4.5, d) >20% clue cells seen on the slide
A vaginal wet prep (wet mount or vaginal smear) is a gynecologic test performed as a STAT (within an hour) on a sample of vaginal discharge used to find the cause of vaginosis, vaginitis and vulvitis. Vaginitis symptoms include itching, burning, discomfort, vaginal discharge, odor and/or rash. It assists in the identification of and diagnosis of vaginal yeast infection, trichomoniasis, bacterial vaginosis, and allergic dermatitis. It may also be used in rape investigations to detect the presence of semen.
How to Perform a Wet Prep:
*Add a drop of specimen (if dry, add saline or sterile water) to a clean slide.
*Add a cover slip and read immediately so the slide doesn't dry out
*Look for clue cells, white blood cells, trichomonas, and yeast (cells, budding, pseudohyphae).
*View under the 40x objective lens, turning down the light source to see the hyaline structures. You may add a drop of KOH (potassium hydroxide) and replace the cover slip to look for fungal elements such as pseudohyphae after looking for the other components on the slide, as the KOH will break down other debris, such as bacteria and cells, leaving only fungal elements if there .
*The image above shows vaginal clue cells covered with bacteria. The edges are no longer visible and the cell looks like sand paper (bottom left). The upper 2 epithelial cells are beginning to be attacked by the mixture of bacteria and you can see the edges beginning to ruffle like a fried egg. Gardnerella vaginalis or Mobiluncus commonly cause the formation of clue cells. Gardnerella vaginalis consists of a mixture of Gram-variable bacteria, such as Gram-positive cocci, Gram-negative coccobacilli, and Gram-negative rods covering the cell. Mobiluncus are curved Gram-negative rods. They may be found along with Gardnerella vaginalis in bacterial vaginosis.
*Lactobacillus (long, slender Gram-positive bacillli/rods) seen on vaginal wet mounts or vaginal Gram-stains is normal, however, and represents good, healthy vaginal flora. You are looking for a mixture of short rods, curved rods, and cocci on the epithelial cells, which cover about 75%-100% of the cell in order for it to be named a "clue cell". When reporting clue cells and bacterial vaginosis, at least 20% of all epithelial cells seen on the slide should be clue cells. A rare clue cell here and there does not truly represent vaginosis. This is in accordance with the CDC standards and Amsel's criterion.
In a normal test, no yeast or Trichomonas will be present on the slide. White blood cells and/or clue cells are usually absent or very low in number. The normal vaginal pH is 3.8-4.5.
Symptoms of Infections Able to be Diagnosed by Wet Mount:
Vaginitis:
Vaginitis is associated with bacterial vaginosis in 40-45% of cases, candidiasis in 20-25% of cases, trichomonas in 15-20% of cases, allergic reactions, dermatitis, herpes simplex virus (HSV), mucopurulent cervicitis, atrophic vulvar vestibulitis, desquamous inflammatory vaginitis, foreign bodies, but is even considered normal in some females.
1) Yeast Infection-thick, white, lumpy, cottage cheese-like discharge; Yeast, buds, and/or pseudohyphae may be present (only seen about half of the time); Other facts:
- Opportunistic vaginal yeast infections (itching, burning, yeasty odor, thick, white discharge, discomfort, sometimes cramping)
- Opportunistic oral thrush infections (white coating inside the cheeks and sometimes on the tongue)
- Candidal onychomycosis (nail or nailbed infections)
- Important cause for morbidity due to systemic infections in immunosuppressed or immunocompromised patients (bloodstream, respiratory, wound, etc...)
- Able to form biofilms on medical devices and equipment
- Commensal oral and gut flora
- Anaerobe
- Flagellate
- Corkscrew motility
- Protozoa (most pathogenic one)
- Causes trichomoniasis (thick green discharge, itching, burning, discomfort)
- Both men and women may be equally infected, however, men tend to be "asymptomatic", therefore, both partners should be treated ("asymptomatic" infections may be as high as 50%!)
- Transmission: skin-to-skin contact via sexual activities; occasionally through shared towels
- Infection: urogenital tract (causes vaginitis in women and urethritis in symptomatic men)
- Epidemiology: Globally, >160 million cases per year, and of that, USA has anywhere from 5-8 million new cases per year
- Symptoms: frothy, foamy, green discharge with a musty/fishy odor; 2% of women also display a "strawberry" (bright red/spotted) cervix with the infection due to the inflammatory response
- Complications: In women who are pregnant, may have increased risk for preterm delivery, low birth weight, increased mortality, predisposition to coinfection with HIV/AIDS due to small abrasions and irritation in the vaginal/uterine/cervical cavities, allowing the tiny viral particles to enter, and cervical cancer; Women may also be at risk for permanent fallopian tube scarring and infertility due to pelvic inflammatory disease (PID); Some infections have been known to travel to the respiratory system, resulting in bronchitis, pneumonia, or oral lesions of the skin mucosa; In men, rare complications have been known to cause an aggressive type of prostate cancer, which may result in mortality (death)
Amsel's Criteria: a) Discharge is thin/homogenous, b) Sample smells fishy upon the addition of KOH (potassium hydroxide)-"Whiff Test", c) Vaginal pH is >4.5, d) >20% clue cells seen on the slide
- Thin, watery discharge
- Fishy odor
- Burning, itching, discomfort
- May occur due to changes in hormones during the menstrual cycle, use of tampons, new sexual partner, imbalances in vaginal pH, or may be due to sexual transmission
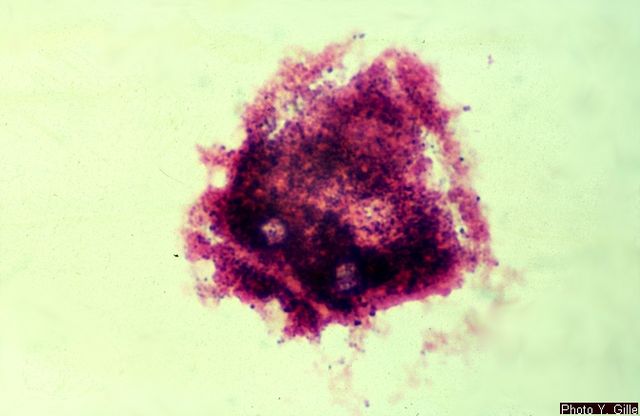
- Clue cells representative of vaginosis, and have a "fried egg" appearance, being covered by a mixture of small GN bacteria (small rods, sometimes curved) and GP bacteria
- Edges of epithelial cells lose their smoothness, and become rough, jagged, and have a ruffled appearance
- Allergy to soaps/detergents/laundry soaps/bubble baths/etc...
- Allergy to latex condoms, powders, spermicides, etc...
- Allergy to various fabrics, such as cotton, polyester, synthetics, etc...
- Allergy to toilet papers or dyes/perfumes/bleaches used in the manufacturing process
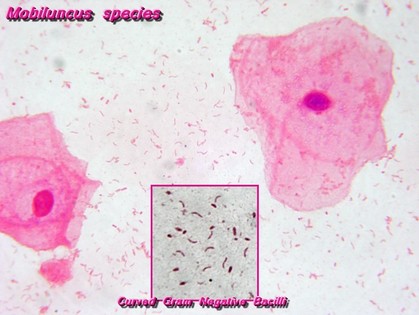
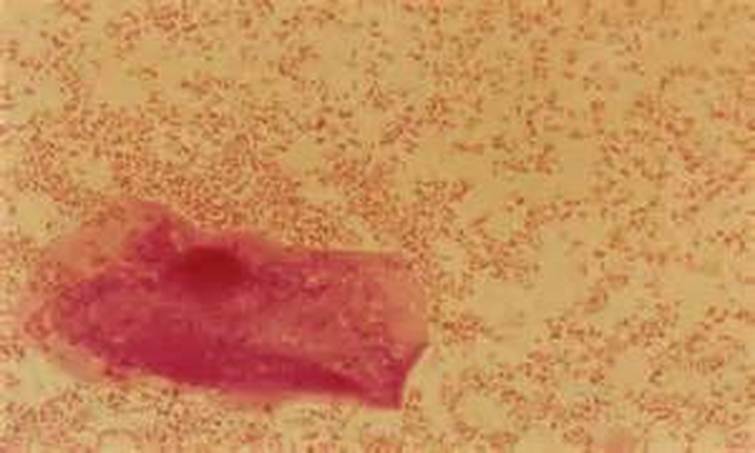
clue cells and mobiluncus spp
Mobiluncus spp may be found in the vaginal tract, but its overgrowth is associated with bacterial vaginosis and it contributes to the formation of clue cells. It is a Gram-variable, small, thin, curved rod and is anaerobic. Tiny colonies form at 48 hours of incubation. It takes 3-5 days for colonies to appear as small, convex, translucent, and low on the plate.
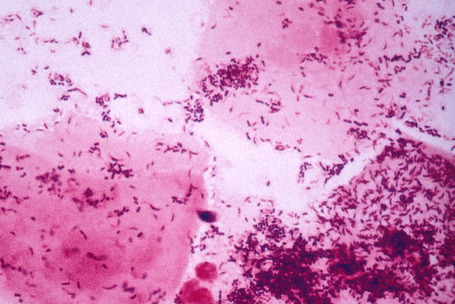
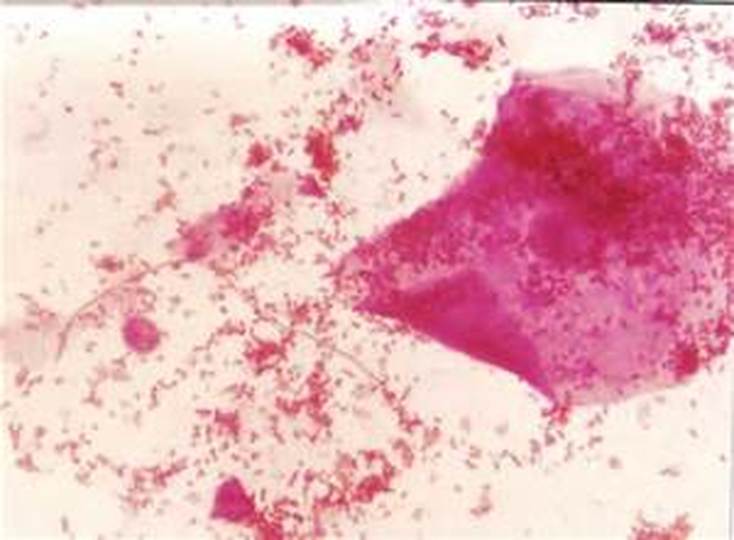
Gardnerella vaginalis and clue cells:
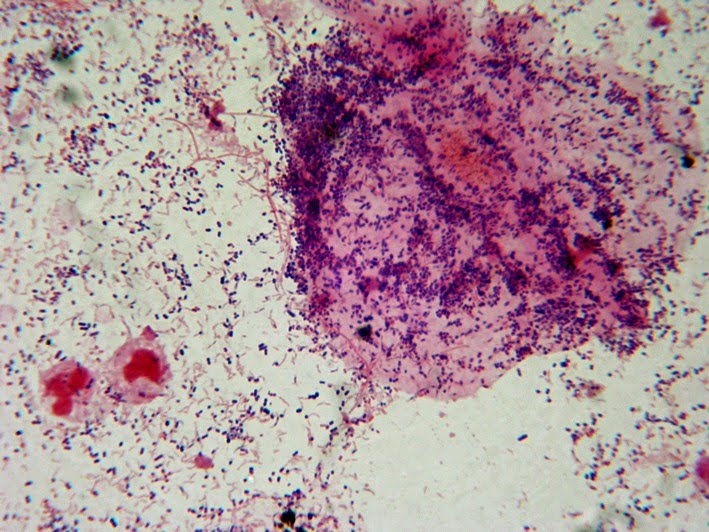
Gardnerella vaginalis is part of the normal vaginal flora of many females, however, its overgrowth is a sign of a disruption of the vaginal pH, contributing to bacterial vaginosis and the formation of clue cells. It is a catalase -, oxidase -, urease -, non-spore-forming, Gram-variable or Gram-negative short rod or coccobacilli (varies in shape, size, color). Virulence factors may include adherence factors and cytotoxin production. It is less commonly associated with urinary tract infections. Bacteremia is very rare but occurs on occasion. Clue cells are squamous epithelial cells that are large with numerous attached Gram-variable small rods and sometimes cocci and coccobacilli. They eat away at the cell, causing it to lose its smooth edges and background, and cells become rough and ruffled like "fried eggs". Large numbers of Gram-positive rods representing Lactobacillus are typically absent or few.
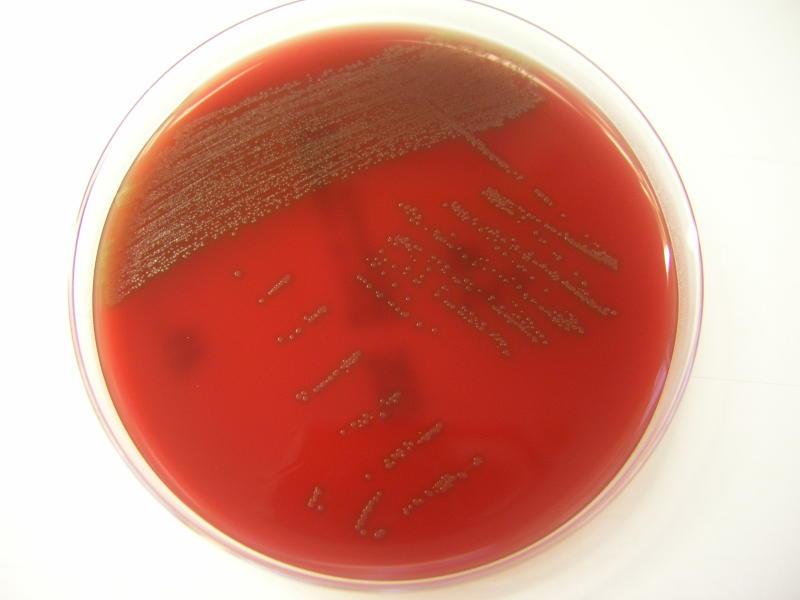
On agar, G. vaginalis appears as small, gray, opaque colonies that are non-hemolytic or slightly green the agar. It is glucose and maltose +, sucrose variable, and typically hydrolyzes hippurate. The drug of choice to treat this organism is metronidazole and it is also susceptible to ampicillin.
On agar, G. vaginalis appears as small, gray, opaque colonies that are non-hemolytic or slightly green the agar. It is glucose and maltose +, sucrose variable, and typically hydrolyzes hippurate. The drug of choice to treat this organism is metronidazole and it is also susceptible to ampicillin.
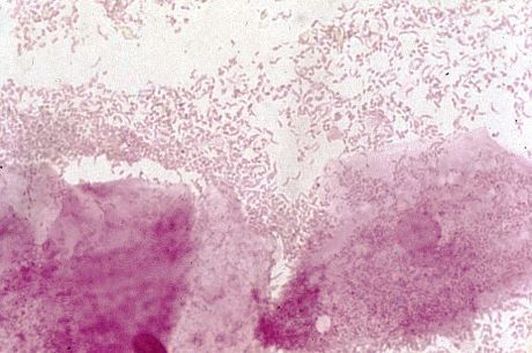
Lactobacillus spp:
Lactobacillus is a catalase -, non-spore-forming, Gram-positive rod that may be pleomorphic, occurring long rods, chaining rods, coccobacilli, or spiral forms. It is glucose, maltose and sucrose +. On blood agar, it appears alpha-hemolytic.
Lactobacillus spp produce lactic acid and they are present in about 42-74% of females. They help to maintain the slightly acidic normal pH of the vaginal environment at 3.8-4.2 pH. It's loss is associated with higher instances of vaginitis, candidiasis, and trichomonas infections.
Lactobacillus spp produce lactic acid and they are present in about 42-74% of females. They help to maintain the slightly acidic normal pH of the vaginal environment at 3.8-4.2 pH. It's loss is associated with higher instances of vaginitis, candidiasis, and trichomonas infections.
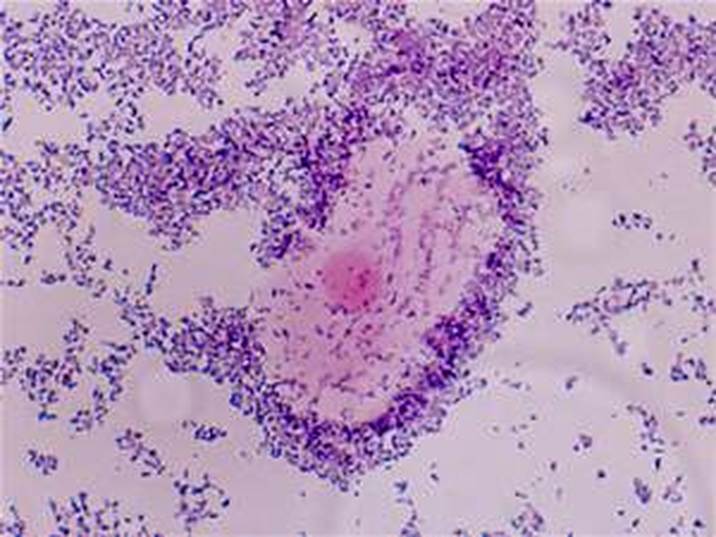
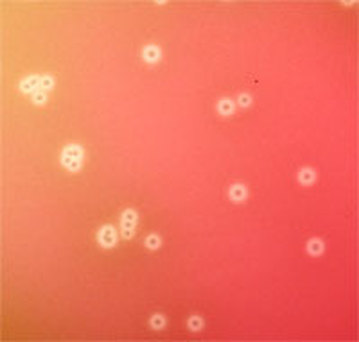
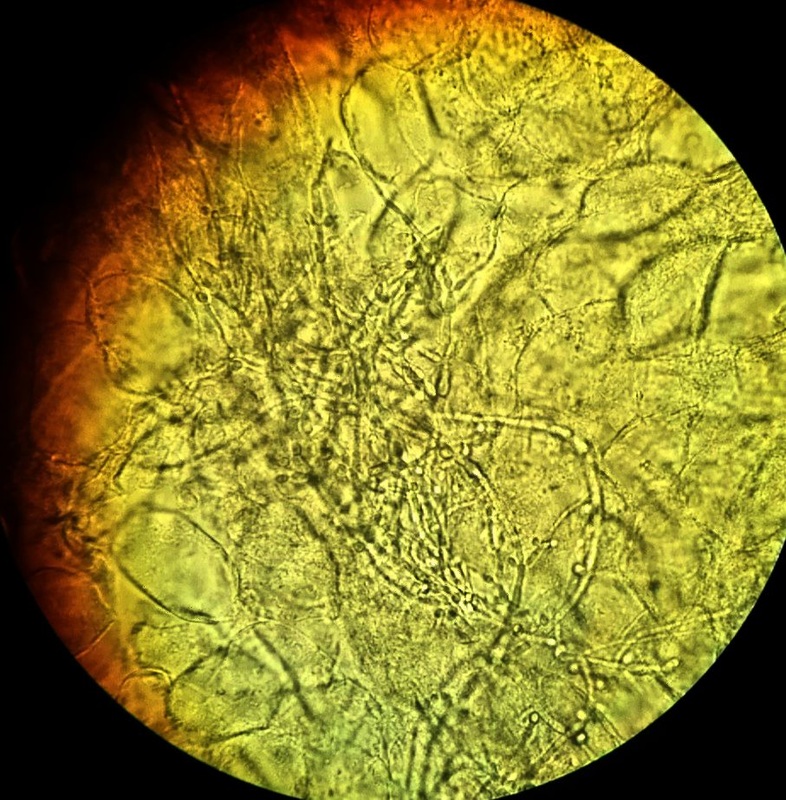
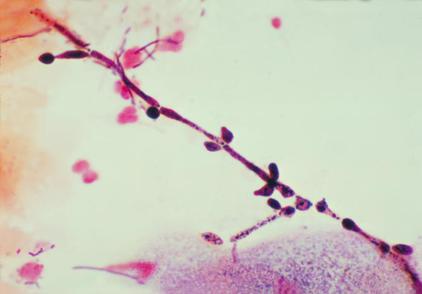
Yeast with pseudohyphae on wet mount
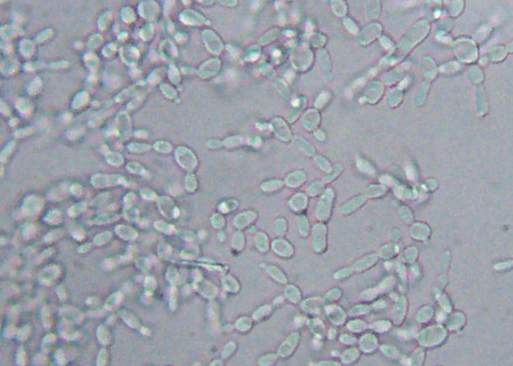
Here is another image of C. albicans in a wet mount exhibiting budding but no pseudohyphae. This yeast is one of the causative agents of vaginitis in women, and patients who are on antibiotics, have diabetes mellitus, who are immunocompromised or immunosuppressed are more at risk for overgrowth of this organism.
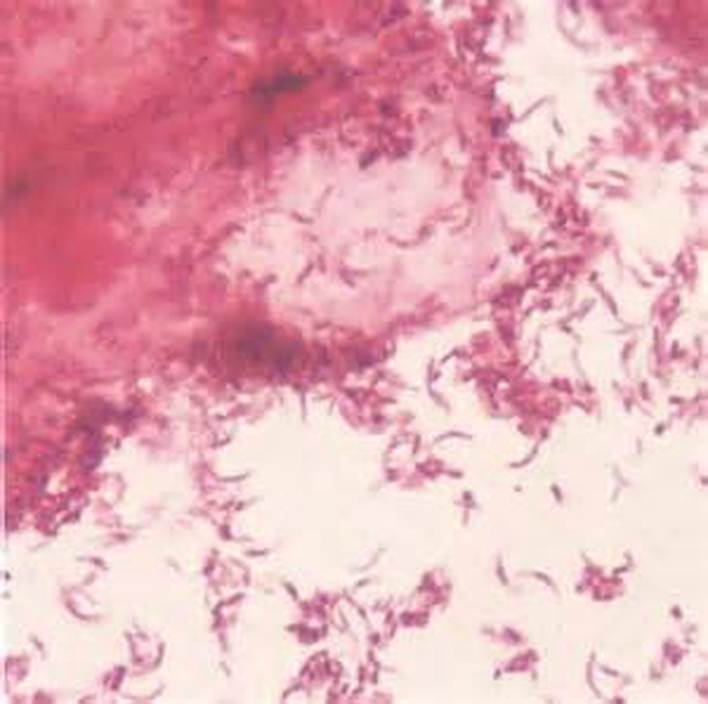
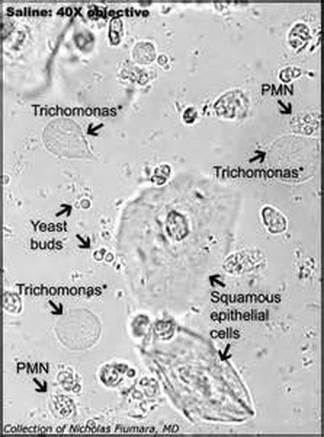
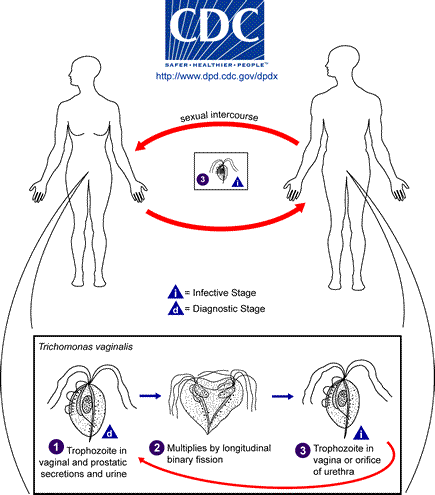
Trichomonas vaginalis
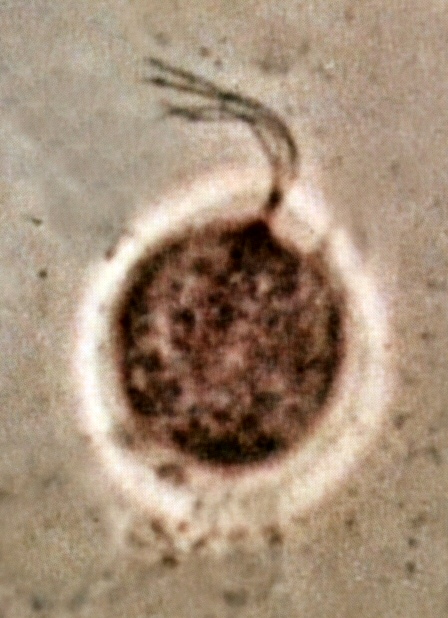
This image shows Trichomonas vaginalis, a vaginal parasite that is motile and exhibits a rapid, darting, zig-zag or dance-like motion due to the presence of flagella. This is one of the causative agents of vaginitis. Both females and males may carry the organism, but males are typically asymptomatic, though they can still transmit the parasite to their female partners.
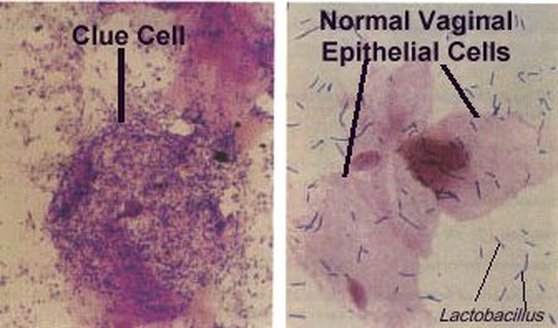
Clue cells (left) covered with numerous mixed bacteria which completely occlude the epithelial cell and normal epithelial cells (right) with healthy vaginal flora (Lactobacillus)
Trichomonas vaginalis
Candida albicans in Gram-stained wet mounts of vaginal secretions showing both pseudohyphae and budding yeast cells. The Gram stain is the gold standard, according to the CDC and Nugent criterion for reporting the budding yeast cells and/or pseudohyphae representative of true vaginal candidiasis.