Introduction to microbiology:
Microbiology: a diverse and specialized area of biology and study of microscopic, living things that cannot be seen with the naked eye and require microscopy for observation; "micro" means small and "ology" is the study of.
Microscopic: cannot be seen with the naked eye; requires a microscope for observation
Microorganisms: living things that can be observed with a microscope:
Host: the individual a microbe lives within or upon
Microbiologist: a scientist, medical lab scientist, clinical lab scientist, medical technologist, medical lab technician, researcher, who studies each aspect of a microbe: cellular structure and function, growth and physiology, genetics, classification, history, interactions with living and non-living things, environment, disease-causing factors, properties they have that may cause disease, etc...
Ubiquitous: exist nearly everywhere
Eukaryote: single-celled organisms with a "true nucleus"
Prokaryotes: do not have a "true nucleus"
Evolution: "evolving" or "changing"; the buildup of changes that occur in organisms as they adapt to their environments
Areas of Microbiology:
Microscopic: cannot be seen with the naked eye; requires a microscope for observation
Microorganisms: living things that can be observed with a microscope:
- Bacteria
- Algae
- Protozoans
- Helminths
- Parasites
- Viruses
Host: the individual a microbe lives within or upon
Microbiologist: a scientist, medical lab scientist, clinical lab scientist, medical technologist, medical lab technician, researcher, who studies each aspect of a microbe: cellular structure and function, growth and physiology, genetics, classification, history, interactions with living and non-living things, environment, disease-causing factors, properties they have that may cause disease, etc...
Ubiquitous: exist nearly everywhere
Eukaryote: single-celled organisms with a "true nucleus"
Prokaryotes: do not have a "true nucleus"
Evolution: "evolving" or "changing"; the buildup of changes that occur in organisms as they adapt to their environments
Areas of Microbiology:
- Medical Microbiology (Clinical Microbiology)
- Associated with the microbes that cause disease in humans and, to some degree, animals
- Bacteriology-study of bacteria
- Virology-study of viruses
- Parasitology-study of parasites and protozoans
- Mycology-study of fungi (yeasts and molds)
- Mycobacteriology-study of acid-fast bacilli, mycobacterium, fungus-like bacteria (actinomycetes, Nocardia)
- Molecular Biology-genetics and PCR
- Processing-receiving, tracking, analyzing, problem-solving, setting up cultures, stains, etc...
- Public Health Microbiology and Epidemiology
- Deals with outbreaks and tracks endemics, epidemics, and pandemics
- Handles reportable organisms
- Monitor the prevention, control and spread of infectious diseases in hospitals and communities, states, the country and the globe
- USPHS
- CDC
- WHO
- Local agencies, such as DHEC
- Research Microbiology
- Examines the factors that cause microbes to be virulent and the mechanisms for inhibiting them (development of antimicrobials, antibiotics, disinfectants, products, antiseptics, etc...)
- Examines the genetics of microbes and their response to their environment
- Develop vaccinations
- Genetic engineering
- Development of recombinant DNA technology
- Veterinary Microbiology
- Associated with the microbes that cause disease in animals
- Immunology or immunoserology
- Studies the body's response to microbes and microbial infection and the complexes and interactions between host cells and the body's immune cells
- Studies principles of vaccination/immunization
- Performs titer testing, immune testing, testing serum and plasma for the presence of antibodies or antigens or a combination of both
- Deals with allergy testing
- Blood testing for a variety of viral diseases
- Industrial Microbiology
- Deals with the safety of our food
- Deals with the safety of our water
- Water testing
- Study and sale and education of water cleaner, water softener, reverse osmosis products
- Includes biotechnology
- Gene therapy
- Study of using plasmids or phages as carriers for new types of therapy
- Bioremediation
- Bread-making
- Beer-making
- Wine-making
- Cheese-making and dairy products
- Vinegar-making
- Fermentation
- Building and making of amino acids, medications, drugs, vitamins, enzymes
- Food inspectors
- FDA
- USDA
- Agricultural Microbiology
- Deals with the relationships between microbes, plants and animals
- Specialized plant specialists or botanists that study plant diseases, soil fertility, soil nutrition and how it affects growth of fruit and vegetables, roots and the nitrogen cycle, plant genetics, cross-breeding, etc...
- Animal specialists that study microbes and how they infect animals
- Environmental Microbiology
- Research the effect of microbes on different habitats, such as desert, tundra, freshwater, saltwater, estuaries, temperate environments, deciduous forests, etc...
- Aquatic and marine biologists
- Soil microbiologists
- Geomicrobiologists
- Astrobiologists
- The study of microbes like algae for bioremediation and biofuels and future medications and other products
The Scientific Method:
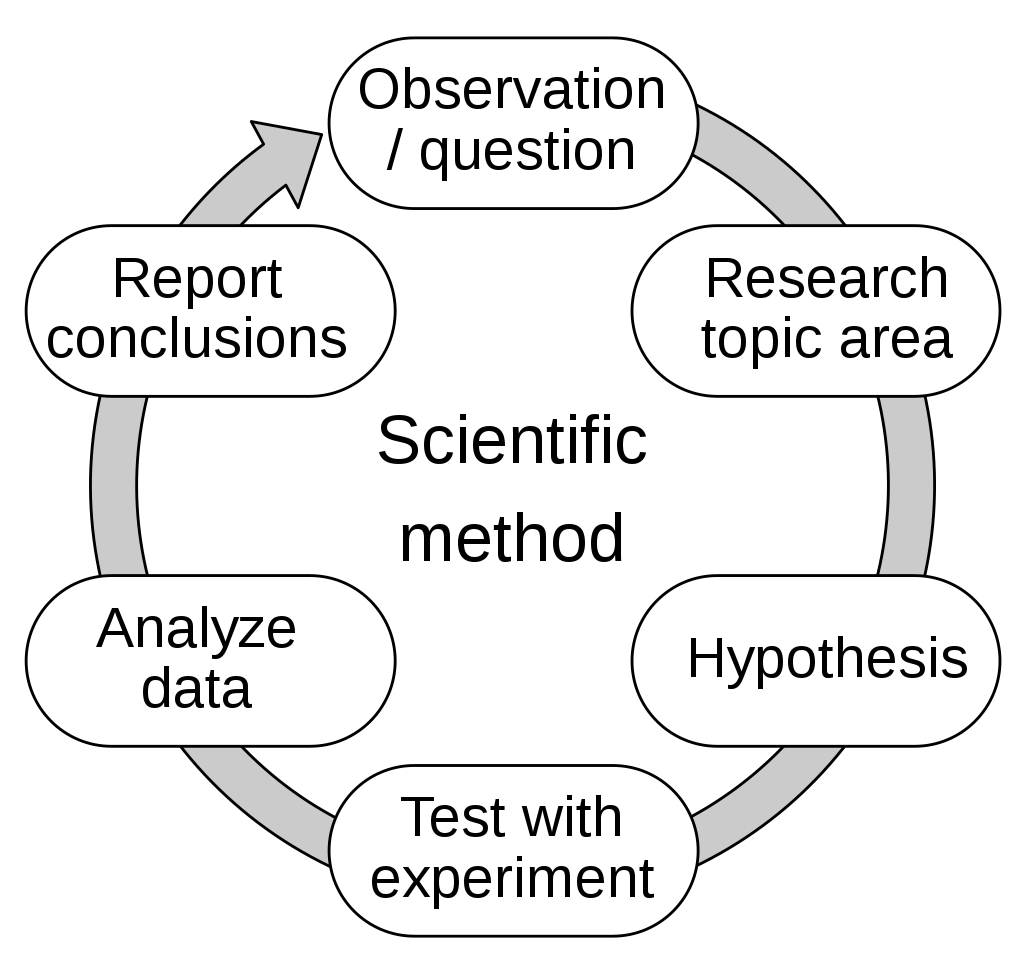
The scientific method is more than just a historical development, it is a lifelong way of thinking and a much-needed foundational tool for anyone, especially those going into the healthcare field, because you will use this day in and day out. This is probably one of the most important concepts you will learn in Microbiology and Biology courses to take into every future course, job, etc...
It begins with making an observation or observations, asking a question or many questions about what you have observed, gathering data and information about your observations and seeking answers to your questions, formulating a hypothesis, testing your hypothesis with an experiment to determine whether it is accurate or correct or not (if not, you can start over again), analyzing your data/results, and then reporting your conclusions.
It begins with making an observation or observations, asking a question or many questions about what you have observed, gathering data and information about your observations and seeking answers to your questions, formulating a hypothesis, testing your hypothesis with an experiment to determine whether it is accurate or correct or not (if not, you can start over again), analyzing your data/results, and then reporting your conclusions.
Phylogeny and Taxonomy:
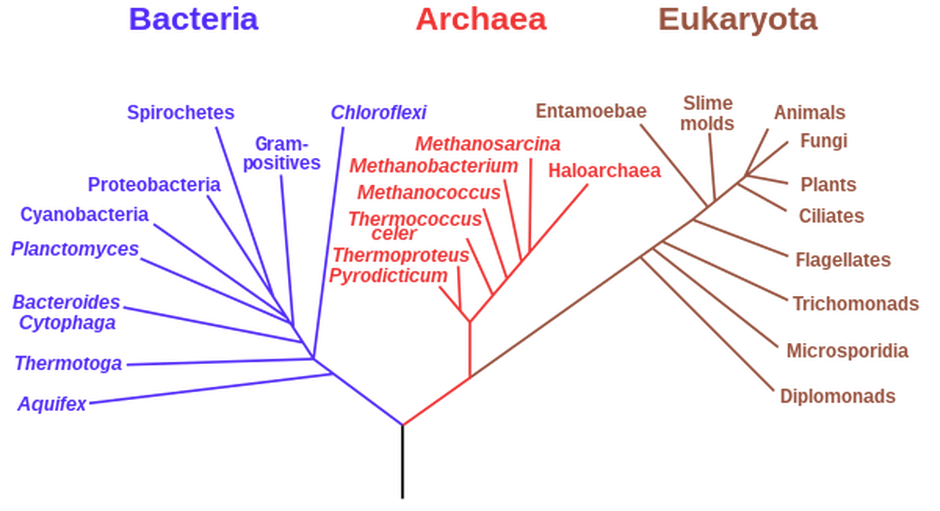
Phylogeny refers to the relationship between organisms. Here, we are looking at the relationships between the 3 major domains of life, developed by Microbiologist and college professor at the University of Illinois Carl Woese, upon his discovery of the 3rd domain of Archaea in 1977. This classification system is still used today. This discovery and classification system played a key role in Woese's part as a founding member of the Institute for Genomic Biology, where research is still conducted today. This system is based on the genetic information of cells, the rRNA, or ribosomal RNA, the cell membrane structure and lipid structure, and finally the cell's response to antibiotics. Believe it or not, microbial life is actually the dominant form of life on Earth.
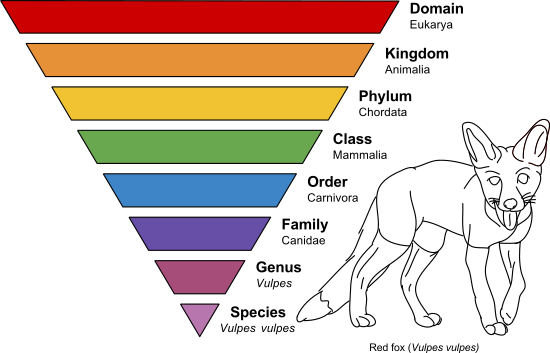
Taxonomy is the study of scientific classification. As seen in the image above, we study Microbiology (the study of microbes) from the level of Domain, Kingdom, Phylum, Class, Order, Family, Genus and Species. This system is how microbes and life are classified. Genus, species are always italicized, and the Genus is capitalized whereas the species is lower case. When we name microbes, whether it be bacteria, fungi, a plant or a parasite, we write them this way. Here are a few examples: Staphylococcus aureus, Escherichia coli, Candida albicans, Aspergillus fumigatus, Penicillium notatum, Naegleria fowleri, etc...
The domains you will be learning about include the following:
Let's begin by looking at Domain Archaea, the oldest, also referred to as "ancient bacteria". There are 2 characteristics that set Domain Archaea apart:
The next domain is Domain Bacteria. They also include prokaryotes. Bacteria are also referred to as "eubacteria" or "true bacteria". These are the prokaryotic cells that are common to humans and the ones we are most familiar with. Clinically significant pathogenic (disease-causing) bacteria fall into this category. They are ubiquitous, meaning that they can be found nearly everywhere. Not all bacteria are pathogenic. Many are good and helpful producers, including producers of antibiotics, they break things down on the Earth, they undergo cycles that maintain plant health and root systems, they provide vitamin K in our gut, which is also a much needed blood-clotting factor, and they are the food digesters in our stomachs. About 97% of bacteria are good and not harmful to the human body. About 2% are opportunistic, meaning that they can cause infection if the conditions are just right and they are in the right place at the right time. And about 1% or less are true pathogens, or infection/disease-causing organisms. Characteristics of bacteria include the following:
Finally, the third domain is Domain Eukarya (Eukaryotes). These are cells with a "true nucleus", cellular organelles and are divided into 4 kingdoms:
Phylogeny refers to the relationship between organisms. Here, we are looking at the relationships between the 3 major domains of life, developed by Microbiologist and college professor at the University of Illinois Carl Woese, upon his discovery of the 3rd domain of Archaea in 1977. This classification system is still used today. This discovery and classification system played a key role in Woese's part as a founding member of the Institute for Genomic Biology, where research is still conducted today. This system is based on the genetic information of cells, the rRNA, or ribosomal RNA, the cell membrane structure and lipid structure, and finally the cell's response to antibiotics. Believe it or not, microbial life is actually the dominant form of life on Earth.
Taxonomy is the study of scientific classification. As seen in the image above, we study Microbiology (the study of microbes) from the level of Domain, Kingdom, Phylum, Class, Order, Family, Genus and Species. This system is how microbes and life are classified. Genus, species are always italicized, and the Genus is capitalized whereas the species is lower case. When we name microbes, whether it be bacteria, fungi, a plant or a parasite, we write them this way. Here are a few examples: Staphylococcus aureus, Escherichia coli, Candida albicans, Aspergillus fumigatus, Penicillium notatum, Naegleria fowleri, etc...
The domains you will be learning about include the following:
- Domain Eukarya (Eukaryotes)
- Kingdom Fungi
- Phylums, etc... will vary depending upon each studied
- Kingdom Protista (Protists)
- Phylums, etc... will vary depending upon each studied
- Kingdom Fungi
- Domain Archaea
- Kingdom Prokarya (Prokaryotes)
- Phylums, etc... will vary depending upon each studied
- Kingdom Prokarya (Prokaryotes)
- Domain Bacteria
- Kingdom Prokarya (Prokaryotes)
- Phylums, etc... will vary depending upon each studied
- Kingdom Prokarya (Prokaryotes)
Let's begin by looking at Domain Archaea, the oldest, also referred to as "ancient bacteria". There are 2 characteristics that set Domain Archaea apart:
- They are prokaryotic cells. (NOTE: some prokaryotes fall under Domain Bacteria as well)
- Archaea cell membranes are unique in that they are composed of branched hydrocarbon chains, some of which contain rings within the hydrocarbon chains.
- The cell membranes are unique because they contain no peptidoglycan.
- Their response to antibiotics varies. They are sensitive to some antibiotics and resistant to others.
- Like the other two Domains, their rRNA is unique.
- They are considered to be extremophiles, because they tolerate harsh environments of extreme heat, extreme cold, extreme CO2, extreme salt levels, extreme pH levels, etc...They have ether-containing linkages that make their membranes very strong and stable, protecting them against extreme heat, cold and acidic conditions.
- Methanogens: extreme methane conditions, like swamps
- Halophiles: extremely salty conditions, like the Great Salt Lake
- Hyperthermophiles: extremely hot temperatures, like at the bottom of the ocean
- Hypothermophiles: extremely cold conditions, like in the ice or glaciers found in Antarctica
- Capnophiles: strong CO2 conditions
- Acidophiles: extremely acidic conditions
- Alkalinophiles: extremely basic conditions (alkaline)
The next domain is Domain Bacteria. They also include prokaryotes. Bacteria are also referred to as "eubacteria" or "true bacteria". These are the prokaryotic cells that are common to humans and the ones we are most familiar with. Clinically significant pathogenic (disease-causing) bacteria fall into this category. They are ubiquitous, meaning that they can be found nearly everywhere. Not all bacteria are pathogenic. Many are good and helpful producers, including producers of antibiotics, they break things down on the Earth, they undergo cycles that maintain plant health and root systems, they provide vitamin K in our gut, which is also a much needed blood-clotting factor, and they are the food digesters in our stomachs. About 97% of bacteria are good and not harmful to the human body. About 2% are opportunistic, meaning that they can cause infection if the conditions are just right and they are in the right place at the right time. And about 1% or less are true pathogens, or infection/disease-causing organisms. Characteristics of bacteria include the following:
- They are prokaryotes.
- They do not have a true nucleus.
- Their cell membranes are made up of unbranched fatty acid chains connected to glycerol heads by ester linkages.
- They are sensitive to some antibiotics and resistant to others, depending on each type of bacteria and the type of antibiotic.
- They contain rRNA that is unique to their species.
- They include Gram-positives, Gram-negatives, cyanobacteria and mycoplasmas.
- Some require oxygen (O2) in order to live (aerobes)
- Some will be killed by oxygen (O2) and require anaerobic conditions (anerobes)
- Some need a little bit of CO2 to survive (capnophiles)
- Some fix nitrogen.
- Some perform photosynthesis and produce O2.
- Some produce antibiotics.
- Some contain plasmids, and can transfer them for antibiotic or disinfectant resistance to other bacteria.
- Most have cell walls that contain either a thick layer or a thin layer of peptidoglycan.
- Some contain lipopolysaccharide in their cell walls.
- Some produce capsules making them difficult to penetrate with antibiotics and enable them to resist the immune system.
- Some produce slime capsules which enable them to glide across surfaces and also make them difficult to penetrate with antibiotics and enable them to evade the immune system.
- Some have flagella (whip-like tails) for movement (unipolar, bipolar, multipolar, peritrichous)
- Some have cilia (hair-like structures) surrounding their surface, which are "hook-like" anchors that enable them to "stick" to mucosal and other surfaces.
Finally, the third domain is Domain Eukarya (Eukaryotes). These are cells with a "true nucleus", cellular organelles and are divided into 4 kingdoms:
- Kingdom Fungi (yeasts, molds and mushrooms)
- Unicellular or multicellular
- Cell walls
- Do not perform photosynthesis
- Absorb nutrients
- Kingdom Protista (protists and parasites)
- Simple and mostly uniecellular
- Slime molds, euglenoids, algae, protozoans (some of these are parasites to humans)
- Kingdom Plantae (plants)
- Multicellular
- Organized into tissues
- Have cell walls
- Obtain nutrients via photosynthesis AND absorption
- Mosses, ferns, conifers, flowering plants
- Kingdom Animalia (mammals, including humans)
- Multicellular
- Organized into tissues
- Lack cell walls
- Obtain nutrients mostly by ingestion
- Do not perform photosynthesis
- Sponges, worms, insects and vertebrates
- They are eukaryotic cells.
- They have a true nucleus.
- They contain specific cellular organelles that perform specific jobs for the cell.
- They have cellular membranes made up of unbranched fatty acid chains attached to glycerol heads, making the interior hydrophobic (water-hating) and the exterior hydrophilic (water-loving) to aid in homeostasis, or balance of water and solutes for the cell
- Not all of them possess a cell wall.
- Those that produce a cell well contain no peptidoglycan.
- They are resistant to antibiotics used for bacteria, but sensitive to most that antimicrobials that affect eukaryotic cells.
- They contain rRNA that is unique to their domain.
What do microbiologists and laboratory technologists/technicians do to isolate and identify bacteria and other microbes?
Microbiologists are Medical Technologists/Medical Lab Scientists and Medical Lab Technicians that work in the clinical laboratory, often separate from the Core Lab, or in research settings and work to culture, isolate a microbe from mixed culture, grow it in a pure culture, then perform tests to identify it. Biochemical tests, immunoassays, rapid polymerase chain reaction (PCR) and mass spectrophotometry, which uses a combination of matrix and proteins and a laser to identify microbes, is also used. Once identified, the microbe is often tested against a panel of antibiotics to see which ones it is sensitive or may be resistant to. This information is entered into the LIS system of the computer so that other healthcare professionals can see the results, or it is called if it is critical. Reportable pathogens are sent to the state public health department, along with special paperwork and a copy of the results/report.
Some important basic terminology regarding microbial cultures include the following terms:
Some important basic terminology regarding microbial cultures include the following terms:
- Culture-one or more types of organisms grown under artificial (in vivo) conditions on an agar Petri dish, slant or broth, at proper temperature and oxygen, no oxygen or slight CO2 conditions, depending upon the culture type.
- Mixed Culture-more than one species is present
- Pure Culture-one species is present; identification requires this and all biochemical and genetic testing is performed from this culture and this is the foundation for all research on infectious disease
- Media/Medium-the material that contains essential resources and nutrients for microbial growth
- Carbon source (sugar)
- Nitrogen source
- Sulfur source
- Other nutrients
- May or may not contain antibiotics to inhibit growth of other organisms
- Gas availability (O2, CO2, etc...)
- May be solid (agar) or liquid (broth)
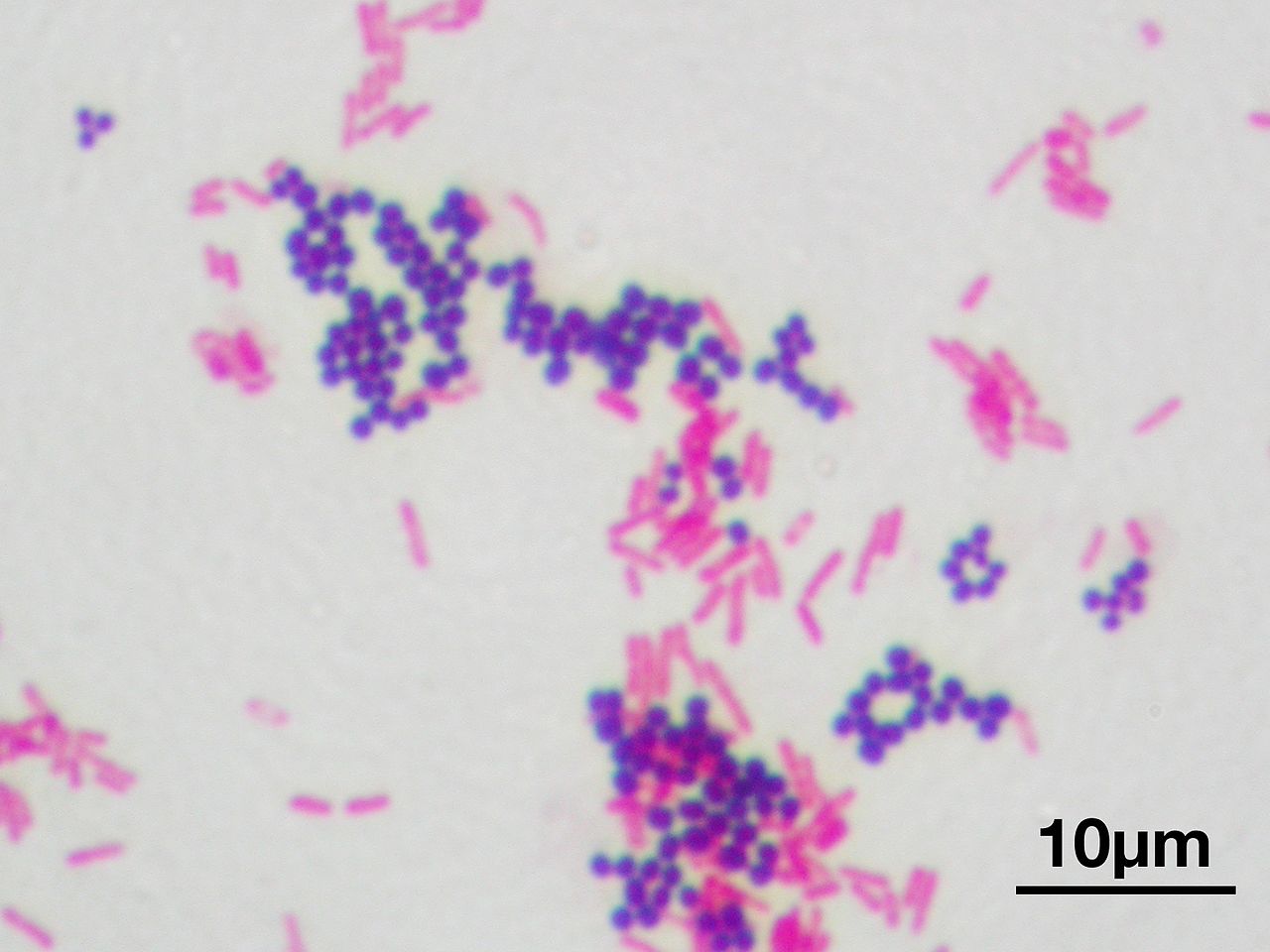
- The Initial Gram-stain-the initial stain performed on samples sent to the lab and the first result healthcare providers will see prior to culturing, growth and other testing so prophylactic (preventative, wide/broad-spectrum) treatment can begin if needed
Isolation Techniques and Selective Media:
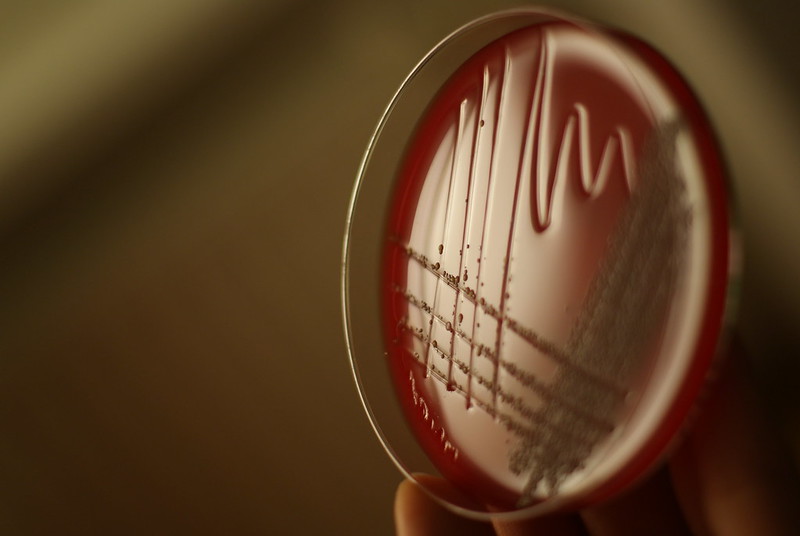
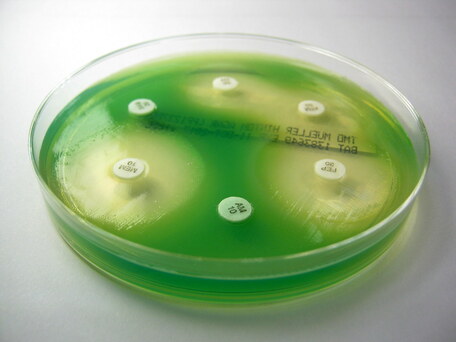
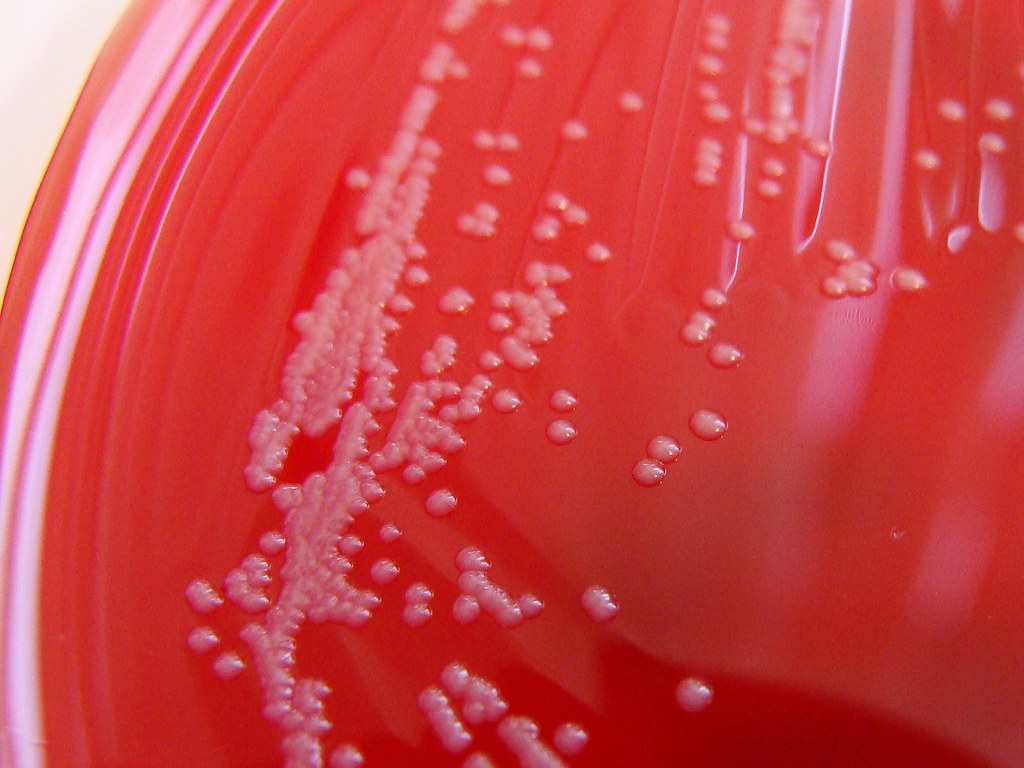
The purpose of the streak plate method of microbial isolation is to obtain a pure culture of that organism. This is critical in order to avoid misidentification, miscommunication and unnecessary treatment for the patient. The streak plate method is the most reliable, but can take time, but it produces individual colonies on an agar plate. A part of an isolated colony may be aseptically collected with a biological loop, either a disposable one or a flamed stainless steel loop, and then transferred to a sterile agar dish or slant or broth to start a pure culture.
Remember, that a microbial culture that has more than one thing growing on it is called a mixed culture. A pure culture contains only a single species. This is why it can take some time to get a result and put it in so that nurses, doctors, PA's and other healthcare workers can see it. Please be patient. We truly do want what is best and right for the patient. This is the gold standard, and it is just the first step in identifying the organism. This commonly used isolation technique is called the streak plate method.
In this method, a bacterial sample is streaked over the surface of a plated agar medium. When the laboratory receives a sample, whether it be a body fluid, blood, tissue, a swab from a throat, ear, eye, wound, respiratory sample, sputum, a BAL, a bronchial brush, etc..., once it is received, tracked to the lab and labels printed with identifiers, this is what happens next. Ideally, these samples are received immediately and plated within 2 hours. With proper PPE and under a biological safety hood, the microbiologist gathers all needed materials and performs the streak plate method. During streaking, the cell density decreases over each of the 4 quadrants, which eventually leads to the individual cells being deposited separately on the surface of the agar. Once cells have been sufficiently isolated, they will grow into groups called colonies that you can see on the plate, each of which consist of the original cell type. They will have different shapes, colors, smells, and characteristics that aid in their identification as well. Since some of the colonies form from individual cells, whereas others form from pairs, clusters or chains, they are referred to as colony forming units (CFU's).
A common streaking technique is the 4-Quadrant Method. This uses a 4-streak pattern on selective media to try to isolate the microbe. This encourages growth of certain microbes while inhibiting the growth of others. There are other types of media that contain indicators, such as color, or bile salts or other nutrients and/or antibiotics that aid in identification and these media types are considered to be selective or differential. I will discuss these further in another section.
Quadrant 1: Streak the plate very "tight" in the first quadrant, holding the plate with one hand and the loop loosely with the other hand.
Quadrant 2: Turn the plate and streak the 2nd quadrant a little bit looser and more spread out. You will start out and cross over into the 1st quadrant to grab some of the bacteria from that quadrant to spread it out.
Quadrant 3: Turn the plate again and streak the 3rd quadrant even more looser and more spread out. You will start out and cross over into the 2nd quadrant to grab some of the bacteria from that quadrant to spread it out.
Quadrant 4: Turn the plate one more time and streak the 4th quadrant as just a squiggle so it is the most spread out and the most loose of all. This is where you will get your most isolated colonies.
Remember, that a microbial culture that has more than one thing growing on it is called a mixed culture. A pure culture contains only a single species. This is why it can take some time to get a result and put it in so that nurses, doctors, PA's and other healthcare workers can see it. Please be patient. We truly do want what is best and right for the patient. This is the gold standard, and it is just the first step in identifying the organism. This commonly used isolation technique is called the streak plate method.
In this method, a bacterial sample is streaked over the surface of a plated agar medium. When the laboratory receives a sample, whether it be a body fluid, blood, tissue, a swab from a throat, ear, eye, wound, respiratory sample, sputum, a BAL, a bronchial brush, etc..., once it is received, tracked to the lab and labels printed with identifiers, this is what happens next. Ideally, these samples are received immediately and plated within 2 hours. With proper PPE and under a biological safety hood, the microbiologist gathers all needed materials and performs the streak plate method. During streaking, the cell density decreases over each of the 4 quadrants, which eventually leads to the individual cells being deposited separately on the surface of the agar. Once cells have been sufficiently isolated, they will grow into groups called colonies that you can see on the plate, each of which consist of the original cell type. They will have different shapes, colors, smells, and characteristics that aid in their identification as well. Since some of the colonies form from individual cells, whereas others form from pairs, clusters or chains, they are referred to as colony forming units (CFU's).
A common streaking technique is the 4-Quadrant Method. This uses a 4-streak pattern on selective media to try to isolate the microbe. This encourages growth of certain microbes while inhibiting the growth of others. There are other types of media that contain indicators, such as color, or bile salts or other nutrients and/or antibiotics that aid in identification and these media types are considered to be selective or differential. I will discuss these further in another section.
Quadrant 1: Streak the plate very "tight" in the first quadrant, holding the plate with one hand and the loop loosely with the other hand.
Quadrant 2: Turn the plate and streak the 2nd quadrant a little bit looser and more spread out. You will start out and cross over into the 1st quadrant to grab some of the bacteria from that quadrant to spread it out.
Quadrant 3: Turn the plate again and streak the 3rd quadrant even more looser and more spread out. You will start out and cross over into the 2nd quadrant to grab some of the bacteria from that quadrant to spread it out.
Quadrant 4: Turn the plate one more time and streak the 4th quadrant as just a squiggle so it is the most spread out and the most loose of all. This is where you will get your most isolated colonies.
Terms Related to Types of media:
Defined Medium-the chemicals and exact amount of all ingredients are known
Undefined, Complex Medium-at least one ingredient is of unknown amount or identity
Selective Medium-contains an inhibitor, whether it be a salt, a color, a pH type, and/or one or more antibiotics that prevent or slow the growth of undesired organisms
Differential Medium-composed in such a manner that it is able to differentiate between organisms (lactose-fermenting, non-lactose fermenting, gas-producing, non-gas-producing, hemolytic, non-hemolytic, alpha-hemolytic, beta-hemolytic, etc...)
Enriched Medium-composed in such a way that they are enriched with special nutrients and factors and/or blood to encourage the growth of specific organisms or in order to encourage patterns of hemolysis
Undefined, Complex Medium-at least one ingredient is of unknown amount or identity
Selective Medium-contains an inhibitor, whether it be a salt, a color, a pH type, and/or one or more antibiotics that prevent or slow the growth of undesired organisms
Differential Medium-composed in such a manner that it is able to differentiate between organisms (lactose-fermenting, non-lactose fermenting, gas-producing, non-gas-producing, hemolytic, non-hemolytic, alpha-hemolytic, beta-hemolytic, etc...)
Enriched Medium-composed in such a way that they are enriched with special nutrients and factors and/or blood to encourage the growth of specific organisms or in order to encourage patterns of hemolysis
Terms related to the common ingredients in selective and differential media and their roles:
pH Indicator-this is a critical key in making a medium a differential type; detects acid or base/alkaline production, depending upon the medium type
Bile salts-oxgall used to select against organisms that cannot survive the acidic environment of the gut, particularly Gram-positive organisms
Lactose-this is the carbon source (fermentable carbohydrate) in media that differentiate between coliforms of the gut and noncoliforms
Thiosulfate-an electron acceptor able to reduce sulfur to H2S gas
Ferric ion-is an indicator of sulfur, and reacts with H2S to form a black precipitate, so colonies will look black on the plate
Bile salts-oxgall used to select against organisms that cannot survive the acidic environment of the gut, particularly Gram-positive organisms
Lactose-this is the carbon source (fermentable carbohydrate) in media that differentiate between coliforms of the gut and noncoliforms
Thiosulfate-an electron acceptor able to reduce sulfur to H2S gas
Ferric ion-is an indicator of sulfur, and reacts with H2S to form a black precipitate, so colonies will look black on the plate
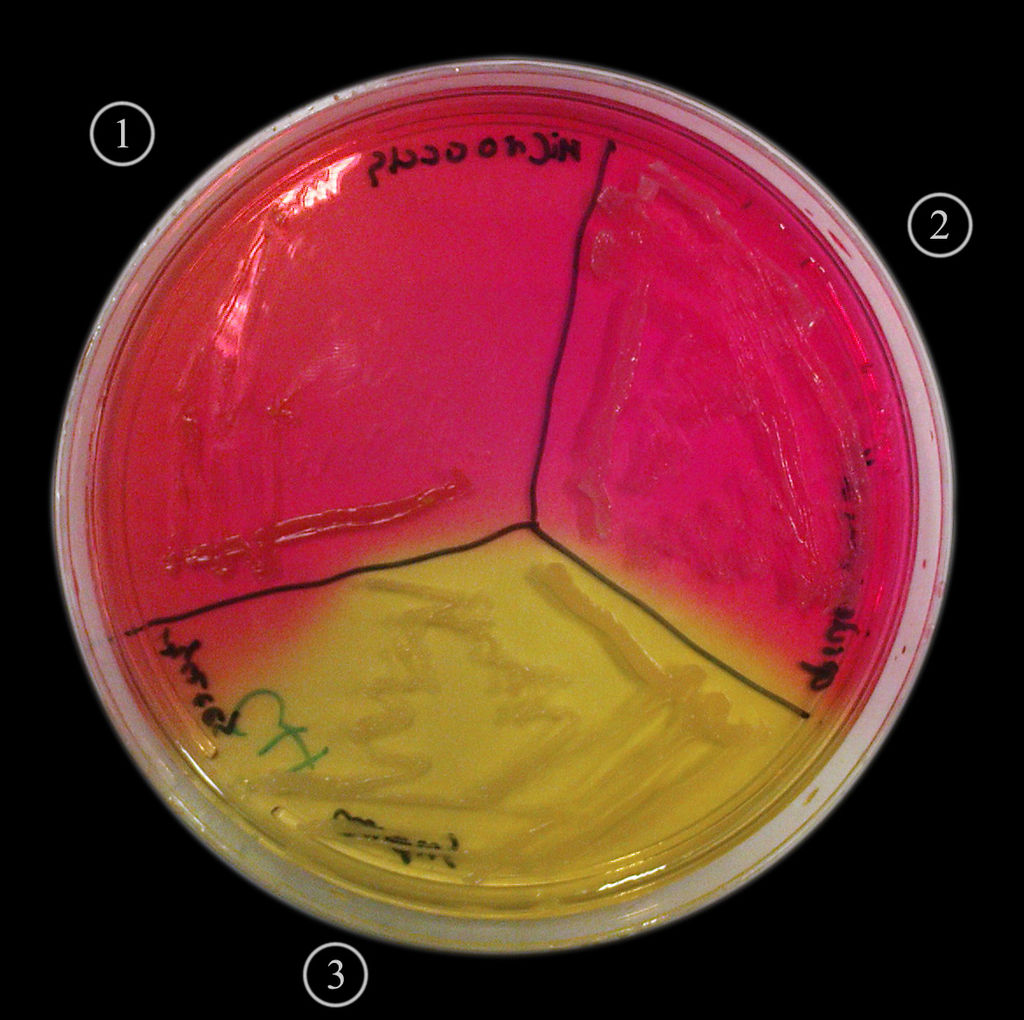
By Navaho - Own work, CC BY-SA 4.0, https://commons.wikimedia.org/w/index.php?curid=5032531; Mannitol Salt Agar is used to isolate and differentiate staphylococci, including S. aureus. It contains mannitol, 7.5% sodium chloride, and the pH indicator phenol red. If the pH is more acidic, <6.8, it is yellow, whereas if it is 7.4 - 8.4, it is red and then it is pink at >8.4. Sodium chloride is selective for S. aureus, since most bacteria cannot survive this high level of salinity. Pathogenic staphylococci ferment mannitol, producing acid, which turns the pH indicator yellow. Nonpathogenic staphylococci also grow on the medium, but do not ferment mannitol, so they remain pink or red.
terms related to organisms themselves:
Enteric-refers to the gut bacteria, typically members of the family Enterobacteriaceae, or Gram-negative rods/bacilli that are able to ferment glucose and share other features in common with each other
Coliform-a member of the enteric family that produces acid and gas from the fermentation of lactose
Noncoliform-a member of the enteric family that does not ferment lactose
Coliform-a member of the enteric family that produces acid and gas from the fermentation of lactose
Noncoliform-a member of the enteric family that does not ferment lactose
Types of media:
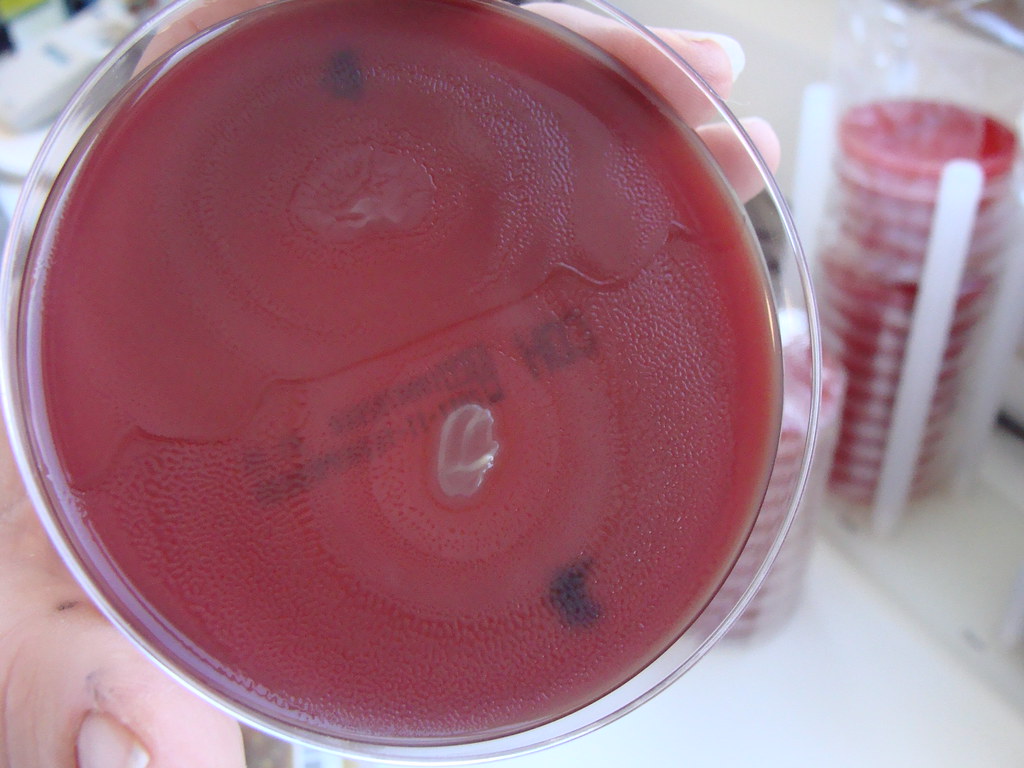
Blood agar (trypticase soy agar with 5% sheep's blood) (sba):
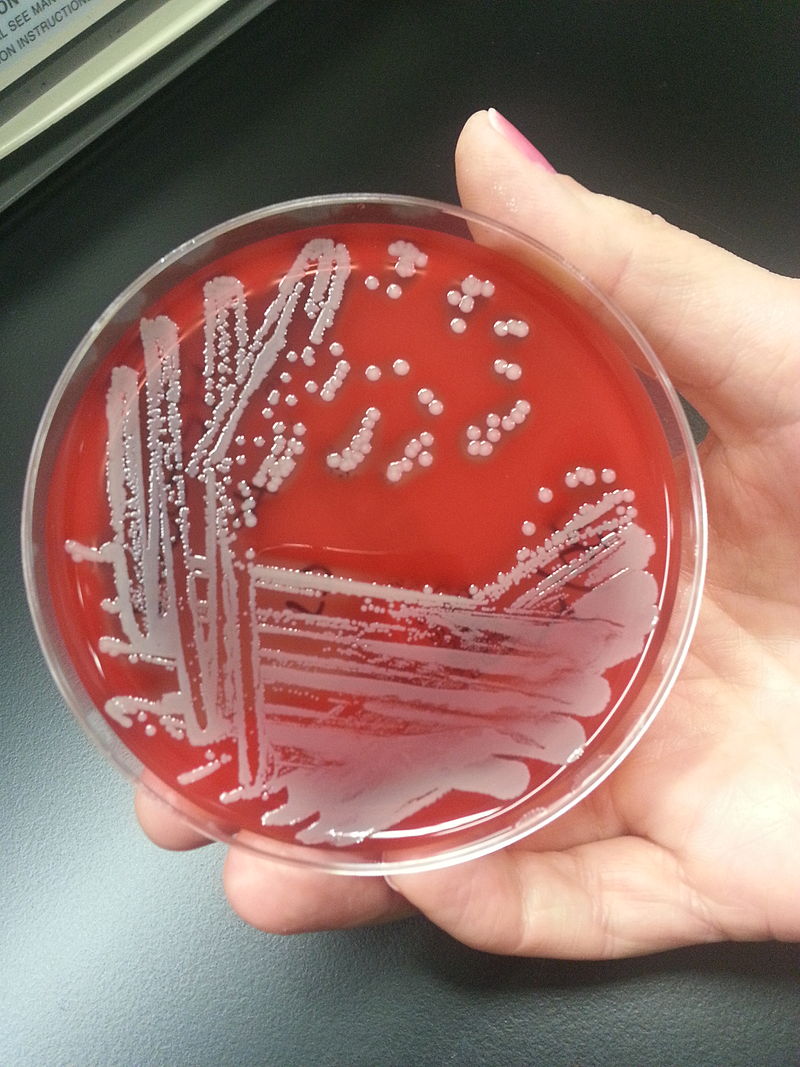
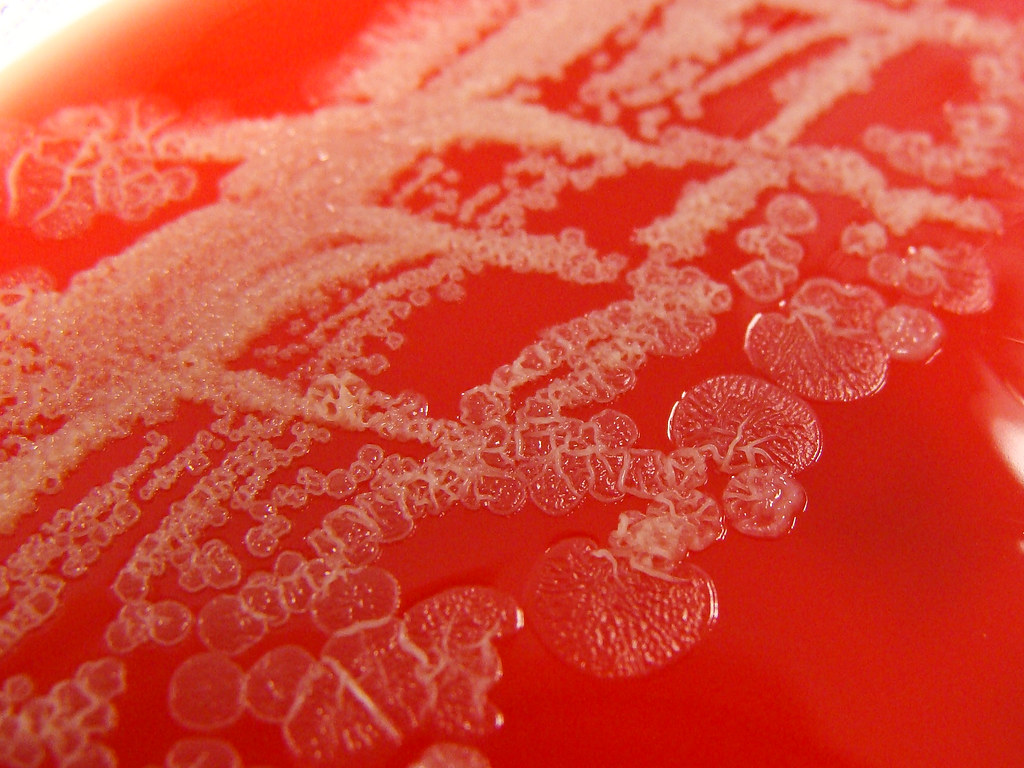
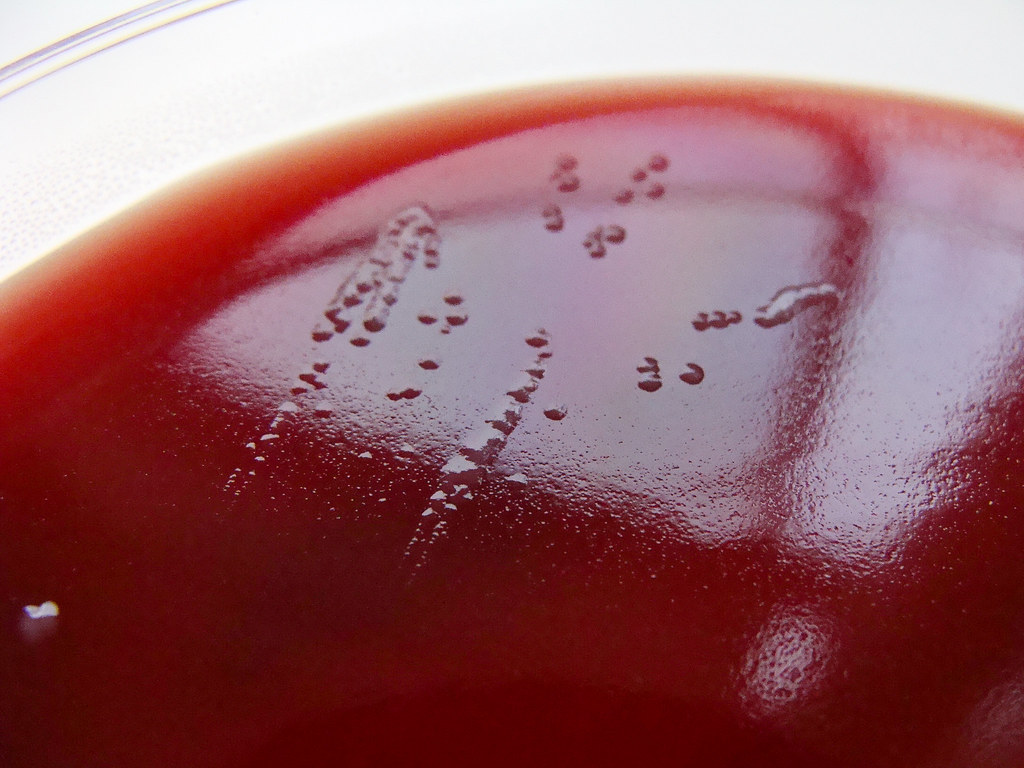
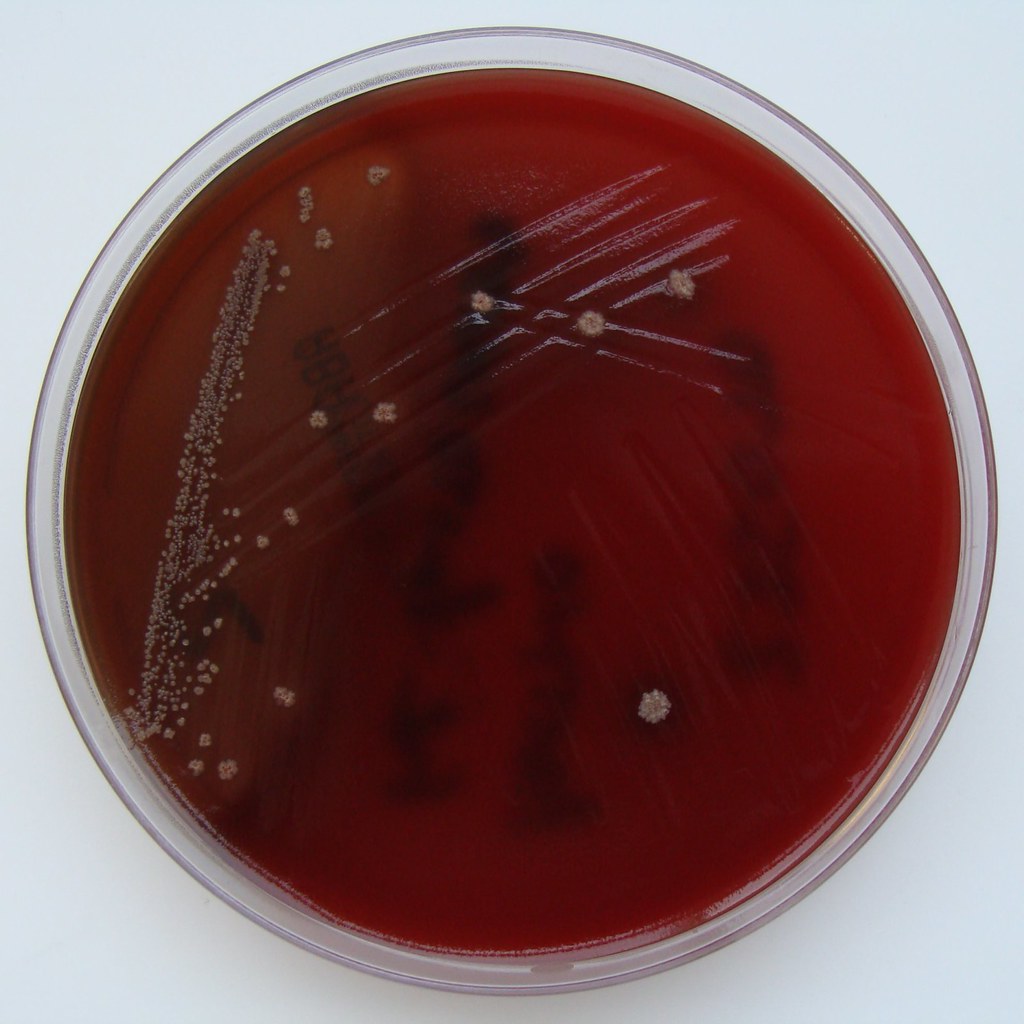
Blood agar is used to isolate and cultivate many types of fastidious bacteria. Fastidious means that they have very specific nutrient requirements in order to grow. Blood agar is used to differentiate bacteria based on their patterns of hemolysis. Streptococcus, Enterococcus and Staphylococcus species have strains that produce hemolysis on the plate, and others that do not. We will look at the patterns of hemolysis.
What causes hemolysis and hemolytic patterns on a blood agar plate? A few species of Gram-positive bacteria produce toxins called exotoxins, specifically referred to as hemolysins. Hemolysins are potent enzymes that "lyse", which means to digest or destroy red blood cells and hemoglobin. Hemoglobin is the iron-binding portion of the red blood cells that carry oxygen throughout the body. both in the human body and on agar that has been enriched with 5% sheep's blood agar. The 5% sheep's blood agar plate has base agar consisting of trypticase soy that has been enriched with 5% sheep's blood, making it red. Bacteria that produce hemolysins make it possible to differentiate bacteria based on their ability to hemolyze, or lyse, red blood cells (or not). There are three major patterns of hemolysis:
Types of hemolysins:
What causes hemolysis and hemolytic patterns on a blood agar plate? A few species of Gram-positive bacteria produce toxins called exotoxins, specifically referred to as hemolysins. Hemolysins are potent enzymes that "lyse", which means to digest or destroy red blood cells and hemoglobin. Hemoglobin is the iron-binding portion of the red blood cells that carry oxygen throughout the body. both in the human body and on agar that has been enriched with 5% sheep's blood agar. The 5% sheep's blood agar plate has base agar consisting of trypticase soy that has been enriched with 5% sheep's blood, making it red. Bacteria that produce hemolysins make it possible to differentiate bacteria based on their ability to hemolyze, or lyse, red blood cells (or not). There are three major patterns of hemolysis:
- B-hemolysis (beta hemolysis)
- The complete digestion/lysing/hemolysis/destruction of red blood cells in the agar and of hemoglobin creates a "halo" or clearing in the agar around the colonies, which can especially be seen if you hold the plate up to the light.
- The complete digestion/lysing/hemolysis/destruction of red blood cells in the agar and of hemoglobin creates a "halo" or clearing in the agar around the colonies, which can especially be seen if you hold the plate up to the light.
- a-hemolysis (alpha hemolysis)
- The partial digestion/lysing/hemolysis/destruction of red blood cells in the agar and of hemoglobin produces a green-to-dark red hue (discoloration) of the agar around the colonies.
- The partial digestion/lysing/hemolysis/destruction of red blood cells in the agar and of hemoglobin produces a green-to-dark red hue (discoloration) of the agar around the colonies.
- y-hemolysis (gamma hemolysis)
- This is actually no hemolysis. There is no "halo", clearing or discoloration around the colonies, so they are normal colonies with no change to the medium.
- This is actually no hemolysis. There is no "halo", clearing or discoloration around the colonies, so they are normal colonies with no change to the medium.
Types of hemolysins:
- Streptolysins (produced by streptococci)
- Type O
- Oxygen-labile
- Produces maximum hemolysis under anaerobic conditions
- Encourage this production by "stabbing" the agar a couple of times in the first quadrant when plating cultures suspected of containing streptococci. The stabs create anaerobic conditions, enabling you to see hemolysis earlier when you have a late-producer or if the plate is mixed and hemolysis is "hidden" under other colonies. This is called the streak-stab technique.
- Oxygen-labile
- Type S
- Oxygen-stable
- Optimal activity under anaerobic conditions
- Oxygen-stable
- Type O
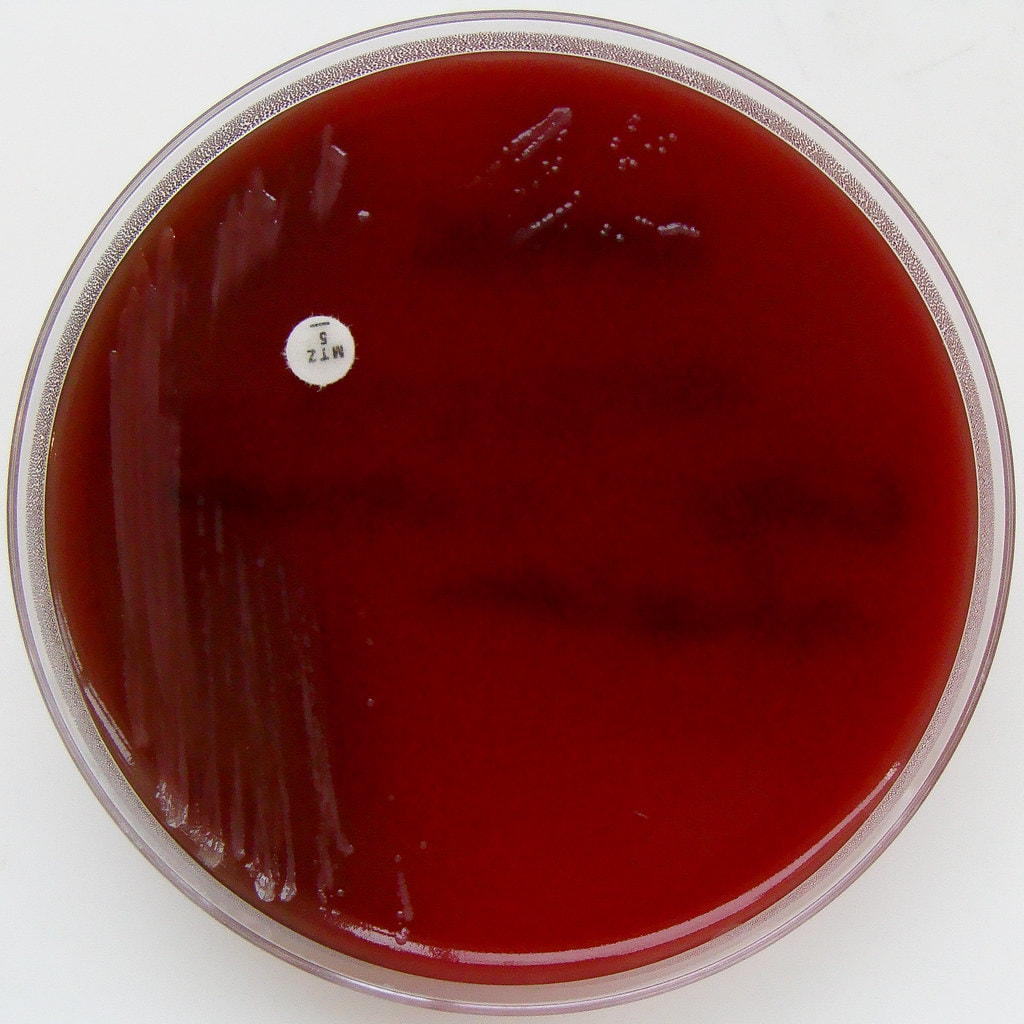
Columbia cna agar with 5% sheep's blood:
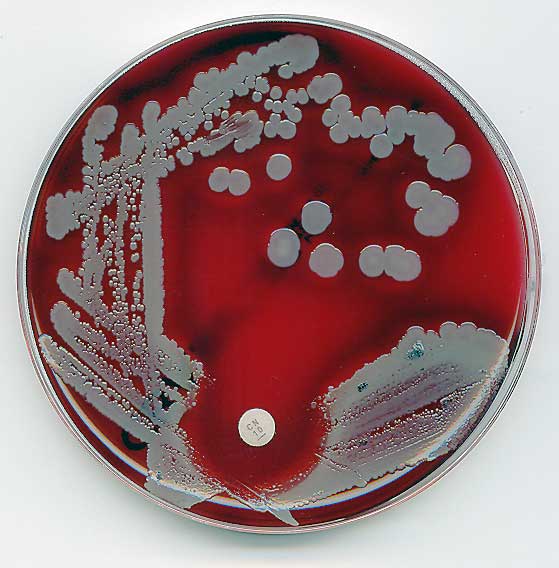
Columbia CNA agar with 5% sheep's blood is useful for the isolation and identification and differentiation of staphylococci, streptococci and enterococci. It is undefined but also a selective and differential medium. It is selective for Gram-positive organisms, but inhibits the growth of Gram-negatives because it contains the antibiotics colistin and nalidixic acid. It also encourages patterns of hemolysis since it contains the 5% sheep's blood. The base agar contains carbon sources as energy, casein, animal tissue, beef extract, yeast extract, corn starch, X factor (heme) and is similar to SBA.
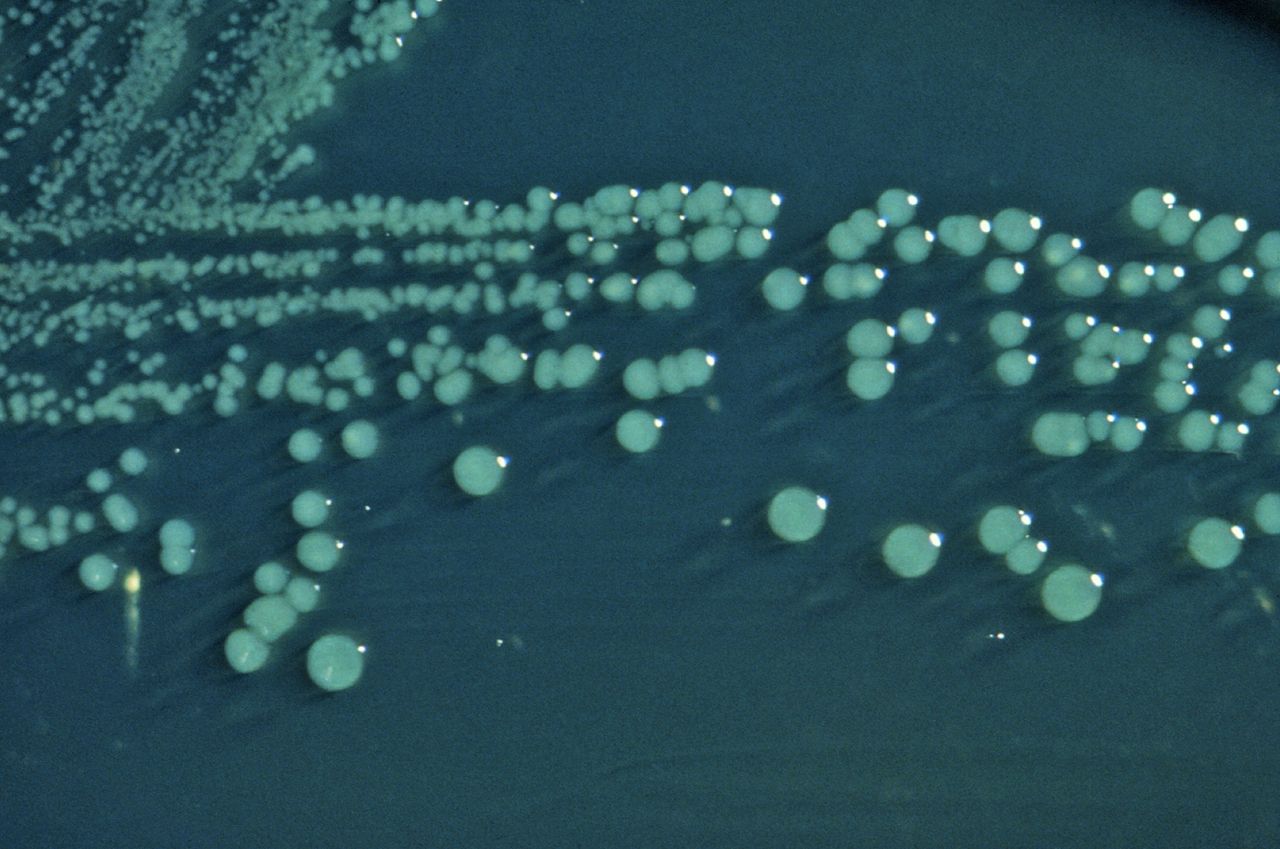
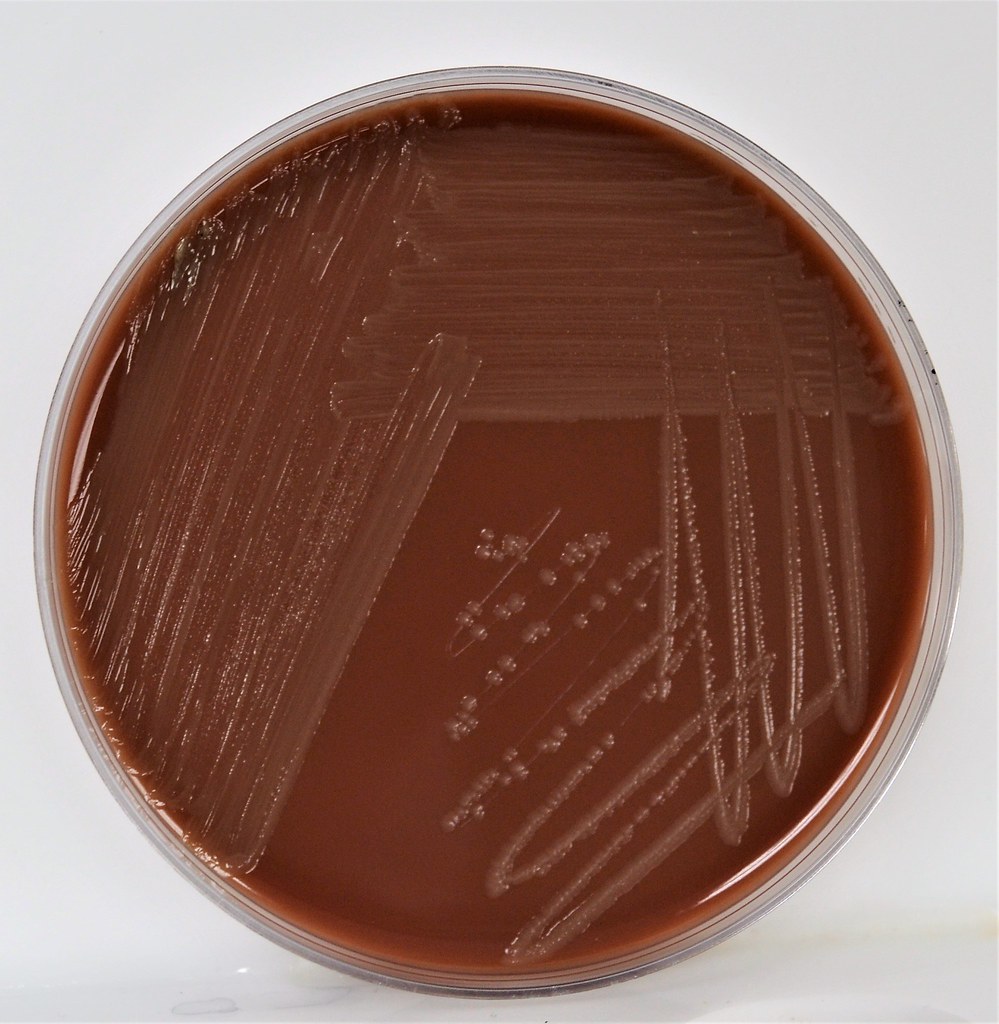
chocolate II agar with horse's blood:
Chocolate II agar is used to isolate and cultivate fastidious bacteria, particularly strains of Neisseria species and Haemophilus species. Chocolate agar has a brown appearance because it is enriched with horse's blood. The base agar consists of peptones, casein, corn starch, phosphate buffer, and bovine hemoglobin. Nucleic acids and amino acids are also added to enrich the agar and encourage growth of Neisseria species. Finally, it is also enriched with 2 blood factors, X and V, which are required by Haemophilus species in order to grow. This medium likes an aerobic incubator at 35-37 degrees with a little bit of CO2. The goal is to isolate Neisseria meningitidis, causative agent of bacterial meningitis, Neisseria gonorrhoeae, causative agent of gonorrhea, and Haemophilus influenzae, causative agent of bacterial pneumonia and respiratory infections, ear infections and eye infections.
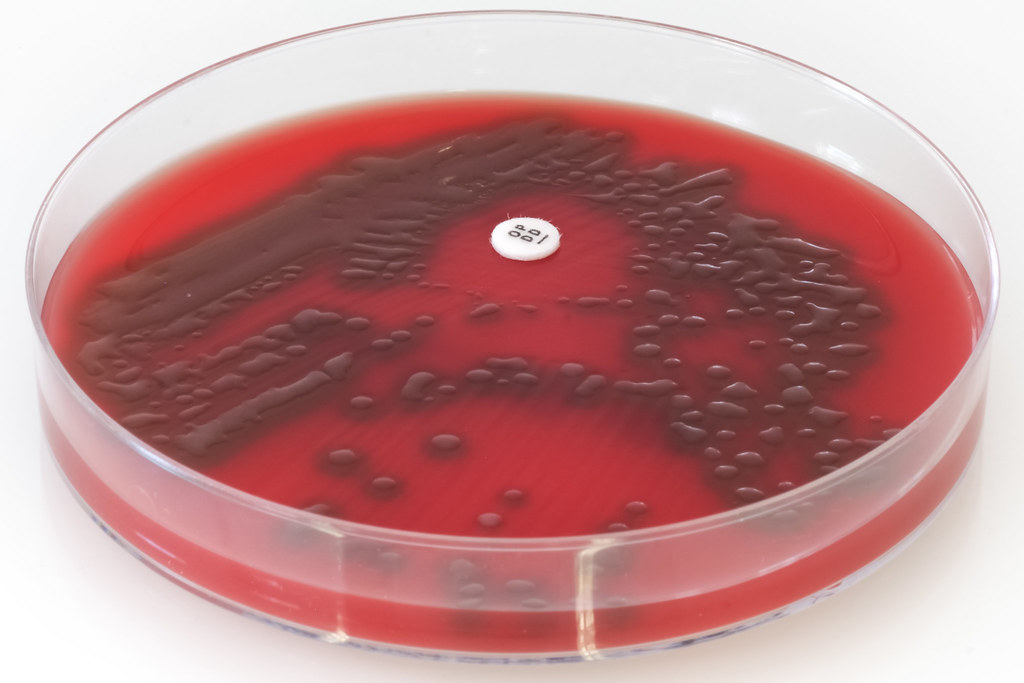
CNA agar with 5% sheep's blood-kv-laked anaerobic agar:
This agar is just like Columbia CNA agar with 5% Sheep Blood Agar, but it is laked with 2 antibiotics: Kanamycin and Vancomycin. It encourages the growth of Gram-negatives such as Bacteroides fragilis and Prevotella species, and inhibits the growth of others. It is selective for Gram-negatives.
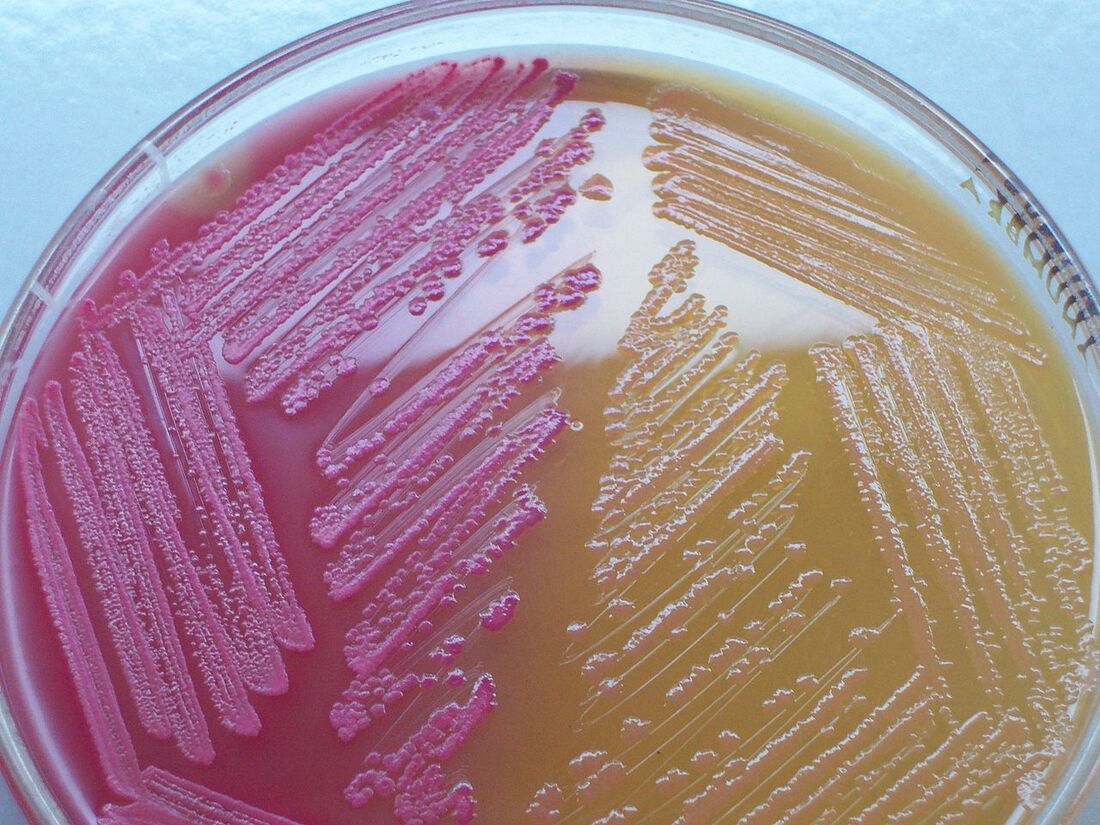
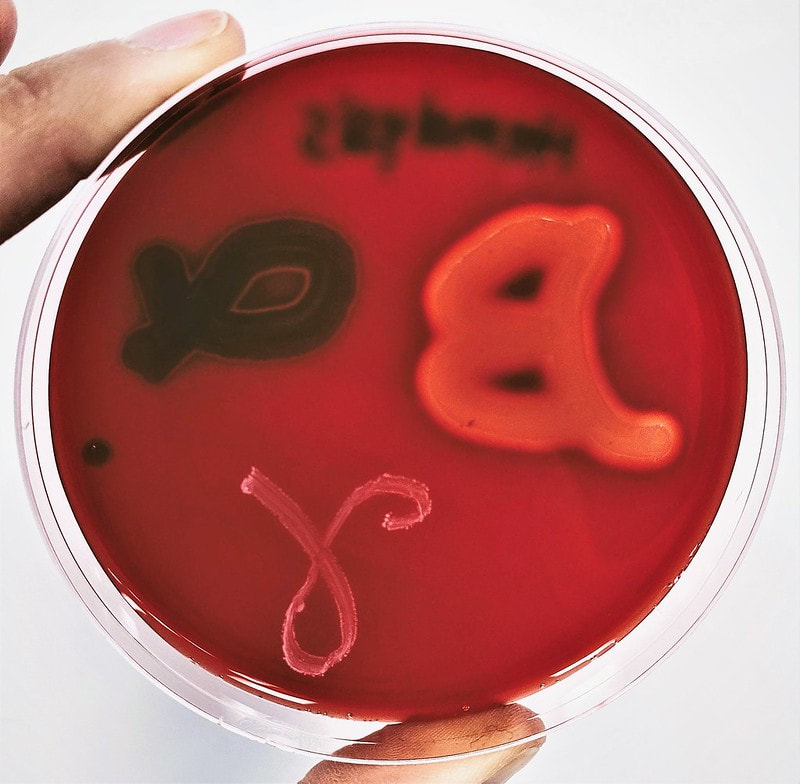
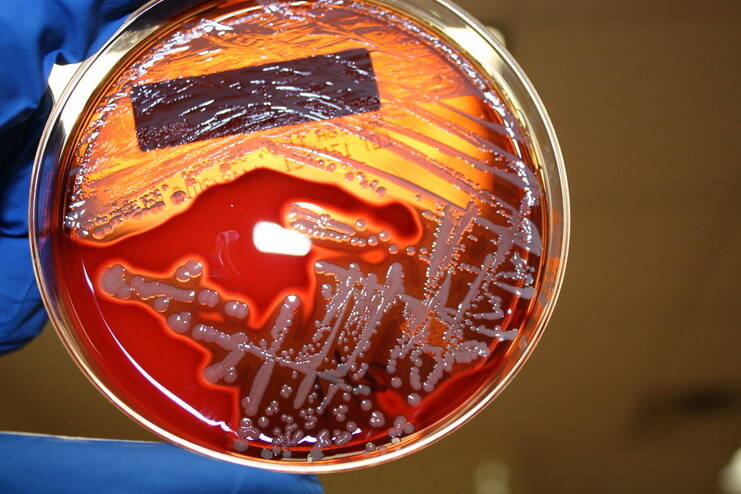
hektoen enteric agar:
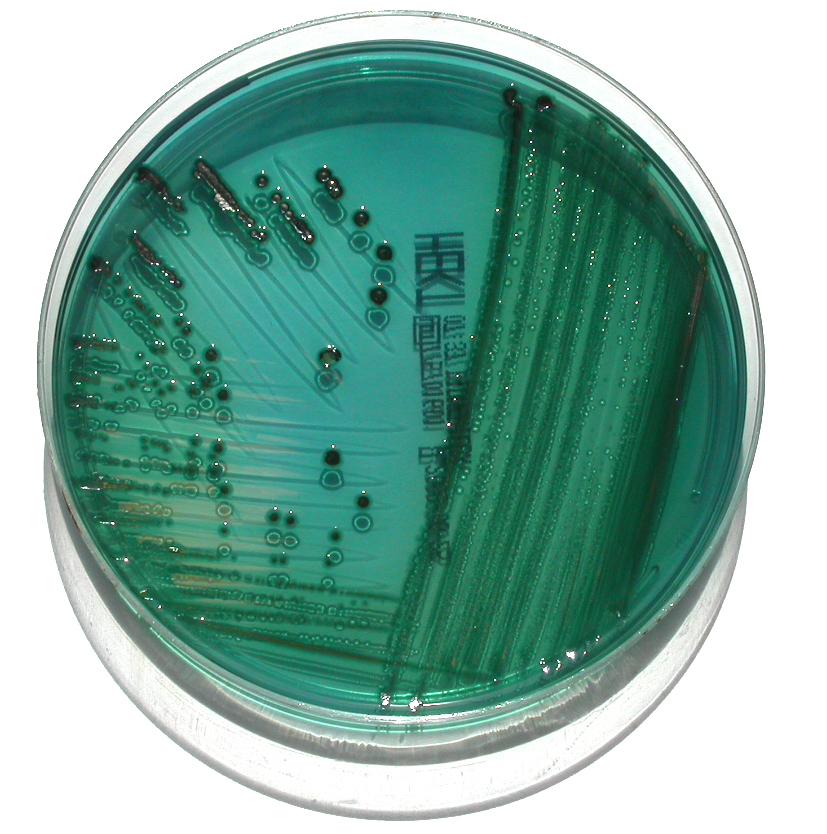
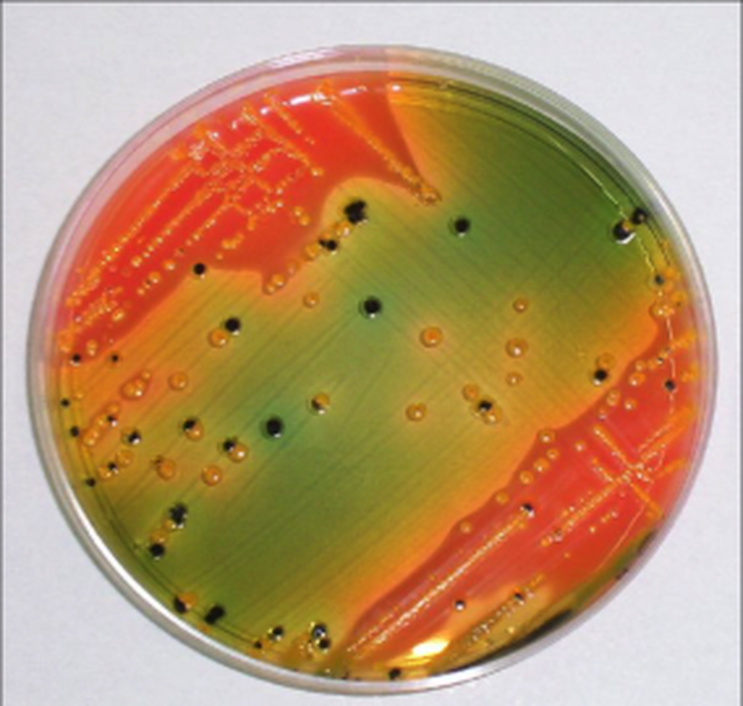
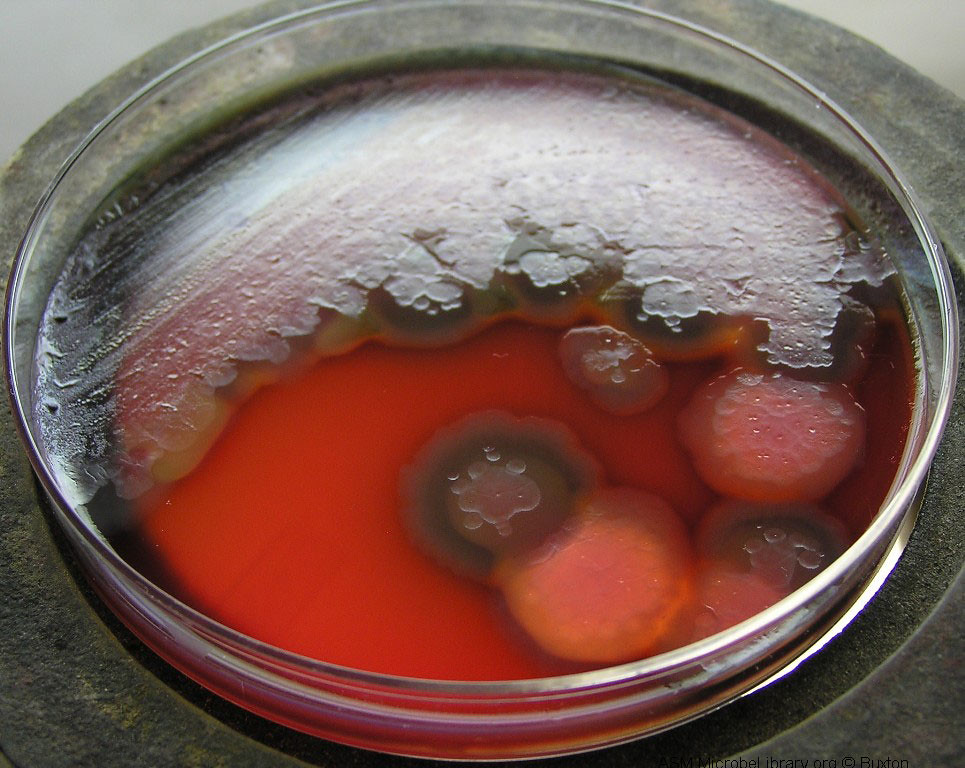
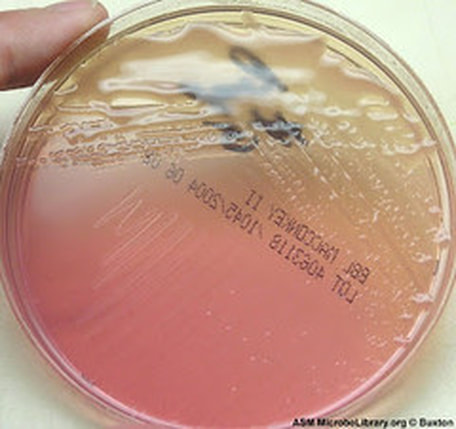
We discussed Hektoen agar a little bit earlier on this page, but this section contains more detail. Hektoen Enteric Agar (HE or HEK) is useful in the identification and isolation of the pathogens Salmonella species and Shigella species from the other Gram-negative Enterobacteriaceae that are normal gut flora. This agar is undefined, and differential. It separates the two pathogens from the other enterics based on their ability to ferment the sugars lactose and sucrose and/or salicin, and to reduces sulfur in the medium to H2S gas. It is also enriched with things like sodium thiosulfate sulfur source), ferric ammonium citrate (reacts with H2S gas and forms a black precipitate), bile salts (block growth of Gram-positive cocci), bromthymol blue (color indicator) and acid fuchsin dye (color indicator). Since different colors will be produced in the colonies and in the agar, this aids in differentiation.
Sugar-fermenters will cause acid to build up in the medium, producing a yellow-orange discoloration in the agar. Those that do not ferment any of the sugars will produce blue-green colonies. Those that reduce sulfur in the medium to H2S gas will produce colonies that contain black precipitate.
Results:
Sugar-fermenters will cause acid to build up in the medium, producing a yellow-orange discoloration in the agar. Those that do not ferment any of the sugars will produce blue-green colonies. Those that reduce sulfur in the medium to H2S gas will produce colonies that contain black precipitate.
Results:
- Yellow-orange colonies and discoloration = normal enteric flora
- Blue-green colonies: produced by Salmonella species, Shigella species, Proteus species, Pseudomonas species
- Black precipitate: produced by Salmonella species, Proteus species
Bacterial and colony growth patterns:
On Agar Plates:
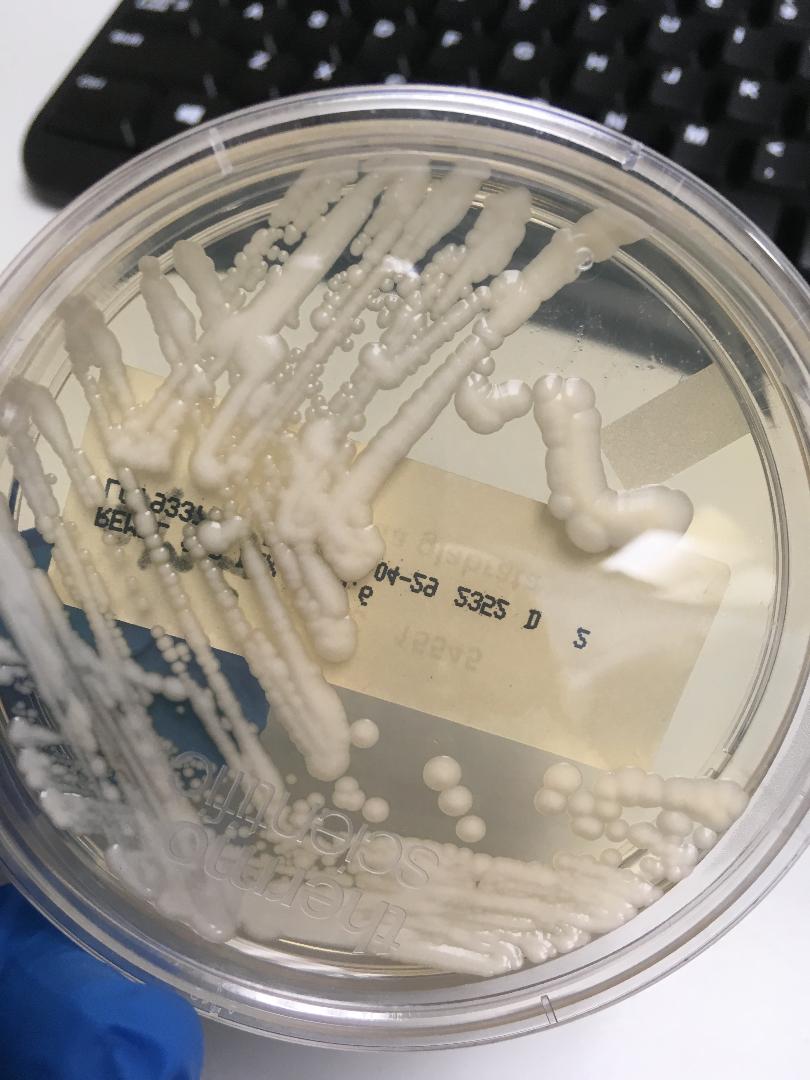
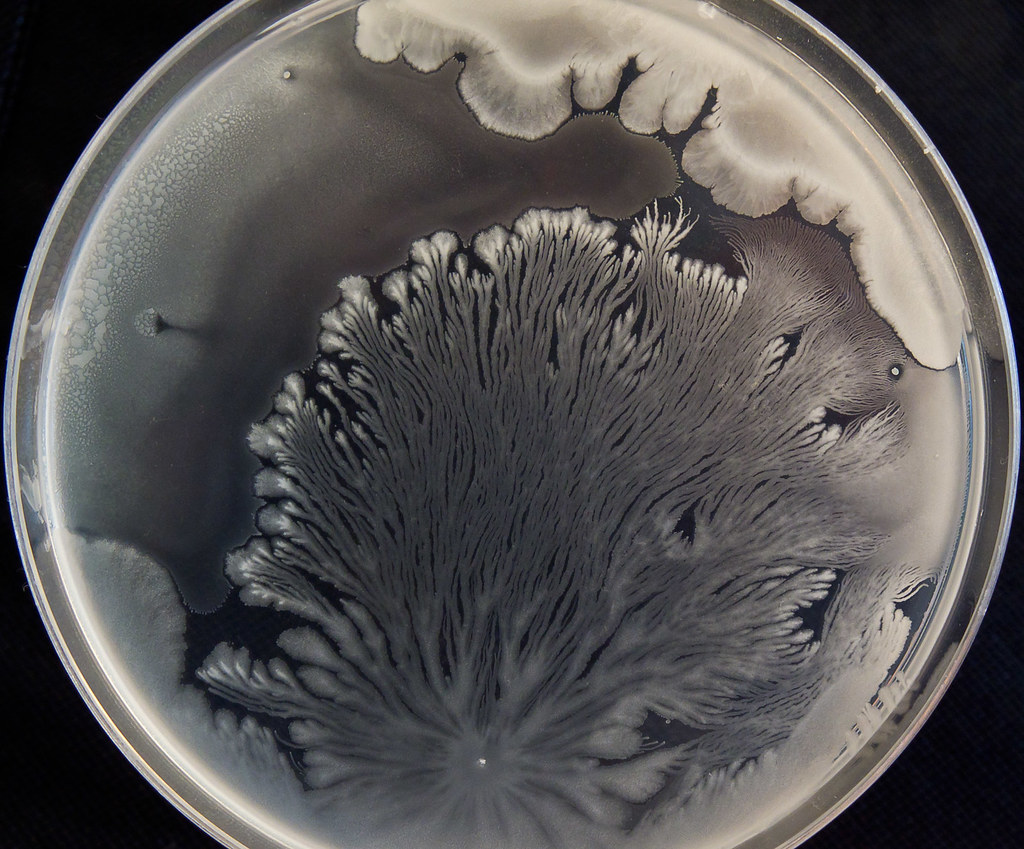
Morphology is the study of bacterial growth. Here, we are looking at the bacterial morphology growth patterns on agar plates and slants. This is just one step in the identification process. Bacteria typically display unique growth characteristics and patterns, colors/pigments and even scents as they grow on agar. Once the bacteria is deposited on the agar and struck across the plate, cells begin to divide at an exponential rate (called the log phase) until a visible colony appears on the surface of the agar. This may take up to 24 hours or longer. From the original plate, once all testing has been performed, a subculture can be performed, transferring the colony of choice to another plate in hopes of isolating a pure culture.
Characteristics of colony morphology include:
Characteristics of colony growth:
Environmental factors that influence bacterial growth include:
In Broth:
In liquid media, also known as broth, bacteria display different patterns of growth than they do on solid media:
Thioglycollate Broth:
GN Broth:
LIM Broth:
In Tubed Solid Media:
Aerotolerance:
Aerotolerance is the bacteria's preference to live with or without oxygen, or whether or not it can tolerate it.
Morphology is the study of bacterial growth. Here, we are looking at the bacterial morphology growth patterns on agar plates and slants. This is just one step in the identification process. Bacteria typically display unique growth characteristics and patterns, colors/pigments and even scents as they grow on agar. Once the bacteria is deposited on the agar and struck across the plate, cells begin to divide at an exponential rate (called the log phase) until a visible colony appears on the surface of the agar. This may take up to 24 hours or longer. From the original plate, once all testing has been performed, a subculture can be performed, transferring the colony of choice to another plate in hopes of isolating a pure culture.
Characteristics of colony morphology include:
- Color
- Shape
- Size
- Texture
- Scent/odor (do not sniff cultures close to your nose)
- Genetic makeup
Characteristics of colony growth:
- Shape
- Round/circular
- Irregular
- Punctiform (tiny)
- Size
- Pinpoint
- Small
- Medium
- Large
- Margin or edge
- Entire or smooth
- Undulate or wavy
- Lobate or lobed
- Filamentous
- Swarming
- Spreading
- Rhizoid or branched-like
- Flat or elevated
- Flat (Example: Clostridium perfringens)
- Raised (most)
- Domed (most)
- Umbonate (button in the middle) (Example: E. coli on blood agar)
- Convex (most)
- Concave or pits the agar (Example: Eikenella corrodens)
- Tooth-like (Example: Actinomyces spp)
- Color
- Golden (Example: Staphylococcus aureus)
- Tan/beige (Example: Klebsiella pneumoniae)
- White (Example: Staphylococcus epidermidis)
- Cream/off-white
- Yellow (Example: Micrococcus luteus)
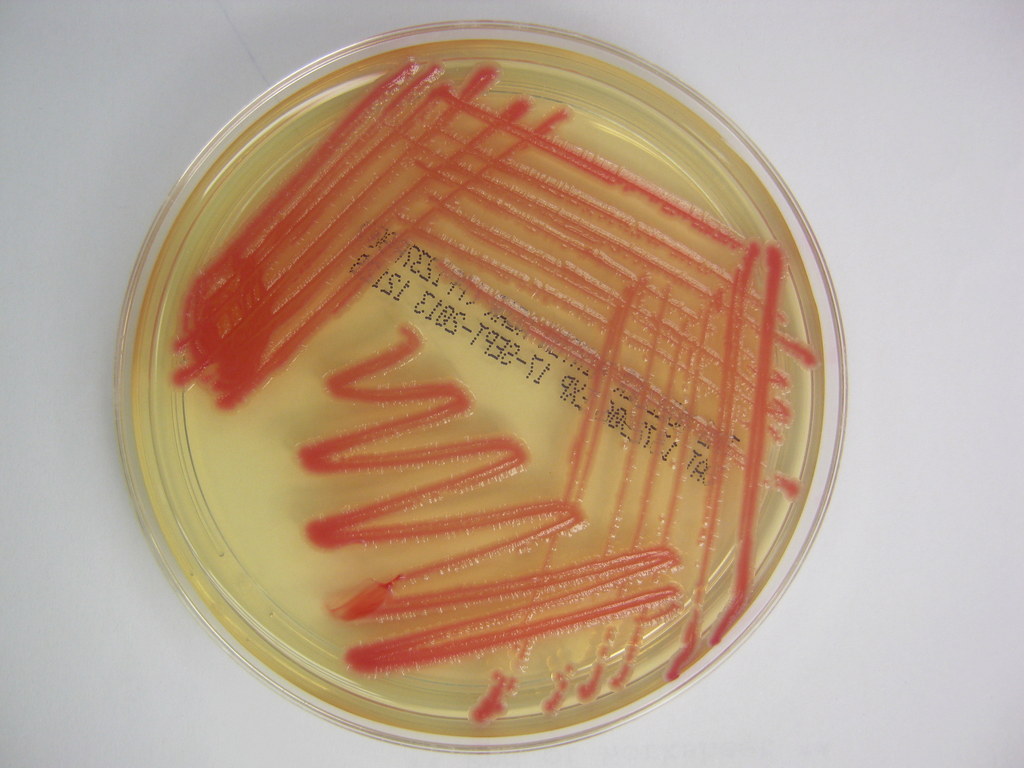
- Red (Example: Serratia marcescens)
- Orange (Example: normal enterics on Hektoen agar)
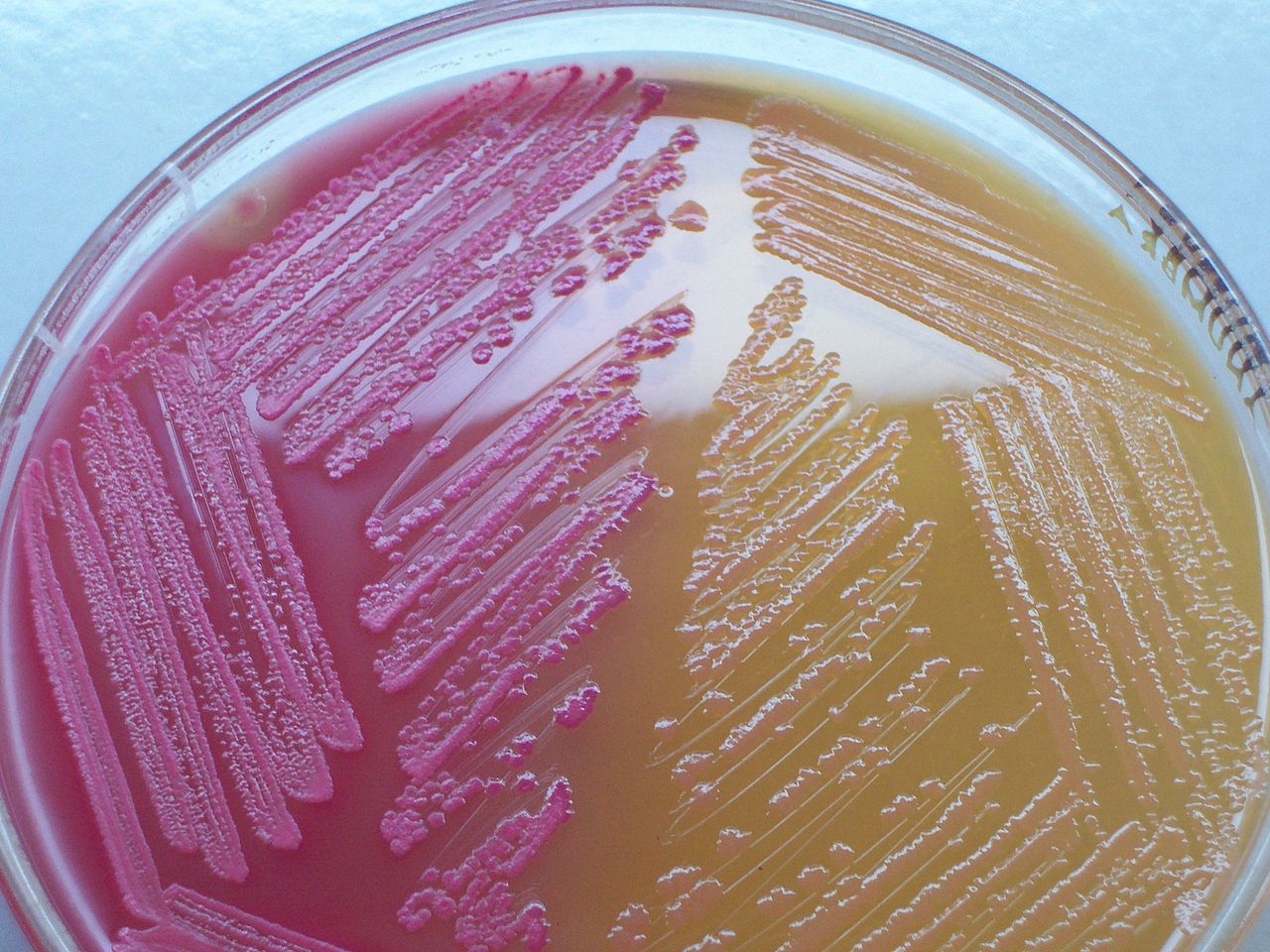
- Pink (Example: Lactose-fermenters on MacConkey agar)
- Black (Example: Salmonella spp on Hektoen agar)
- Gray (Example: Enterococcus faecalis)
- Green (Example: Proteus spp on Hektoen agar)
- Blue-green (Example: Shigella spp on Hektoen agar)
- Black centers (Example: Salmonella species on Hektoen agar)
- Lactose-fermenting (Example: E. coli on MacConkey agar)
- Opaque
- Translucent (Example: Finegoldia magna on anaerobic agar)
- Transparent (Example: Pasteurella multocida on blood agar)
- Shiny (Example: Staphylococcus epidermidis on blood agar)
- Matte (Example: Bacillus subtilis on blood agar)
- Metallic (Pseudomonas aeruginosa)
- Brick red (Prevotella species)
- Fluoresce (some Prevotella spp fluoresce under UV light)
- Texture
- Creamy
- Moist
- Mucoid
- Dry
- Crumbly
- Wrinkled
- Double
- Glistening
- Patterns of Hemolysis
- B-hemolysis
- a-hemolysis
- y-hemolysis
- Scent/Odor
- Flowery/floral (E. coli)
- Pungent
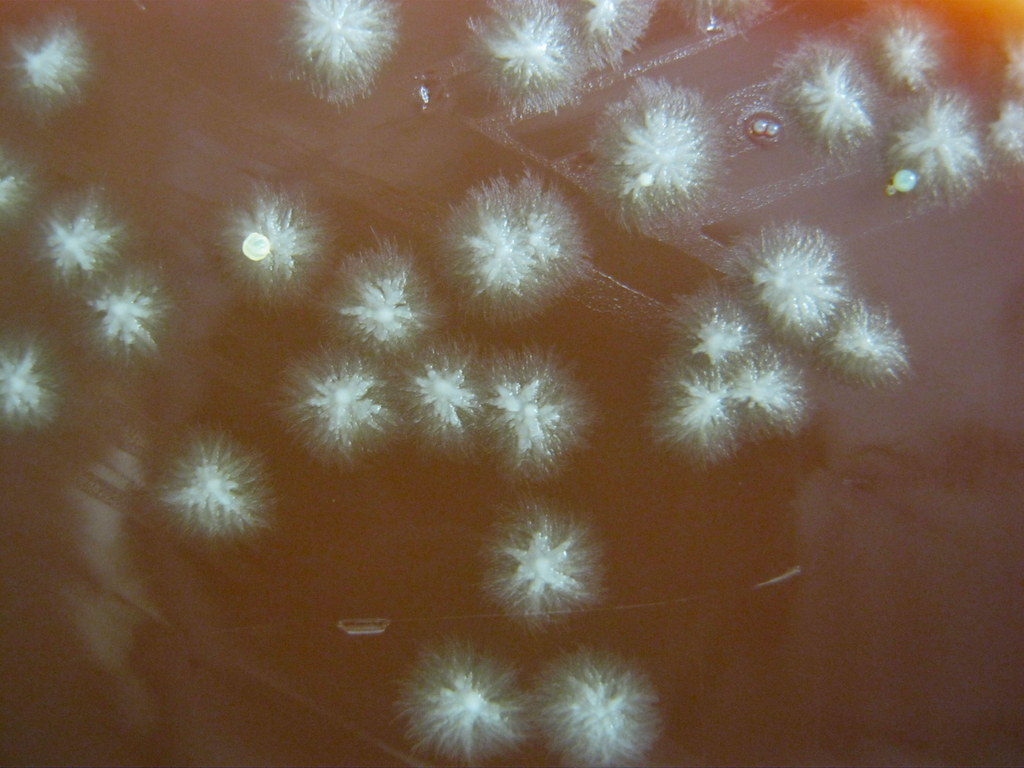
- Musty or like dirt (Actinomyces, Nocardia)
- Bleach (Eikenella corrodens)
- Fruity (Pseudomonas aeruginosa)
- Rancid like rotten grapefruit
- Chicken soup (Proteus mirabilis)
- Dirty gym socks (Proteus vulgaris, Citrobacter, Enterobacter, Klebsiella, Acinetobacter, Providencia)
- Diaper pee (Klebsiella pneumoniae)
- Bread or beer (Candida albicans)
Environmental factors that influence bacterial growth include:
- Temperature
- 35-37 degrees Celsius
- 42 degrees Celsius
- Incubation Time
- 24 hours
- 48 hours
- 72 hours
- 96 hours
- 5-7 days
- 30 days
- 3 months
- Carbon source(s)
- Lactose
- Sucrose
- Dextrose/glucose
- Maltose
- Other
- Requirements for O2 (or not)
- Aerobic (Ambient/O2)
- Anaerobic (No O2)
- Requirements for CO2 (or not)
- Capnophilic (CO2 incubator)
- Availability of nutrients
- Each agar dish/media type is unique
- Moisture/humidity
- Water buckets are put in the bottom of incubators to create a moist environment
In Broth:
In liquid media, also known as broth, bacteria display different patterns of growth than they do on solid media:
- Some float on the top of the medium as a surface membrane (pellicle)
- These are nonmotile
- Often have a waxy cell wall
- Some sink to the bottom of the broth (sediment)
- These are nonmotile
- Some clump together in the broth (flocculence)
- Some grow evenly throughout the broth and cause it to appear cloudy (uniform fine turbidity)
- These are motile
- Some produce pigments
Thioglycollate Broth:
- Used to cultivate anaerobic or microaerophilic bacteria
- Simple
- Inexpensive
- Basic or enriched with supplements
- Yeast extract, casein, dextrose, sodium thioglycollate, L-cystine, resazurin
- Turns pink when oxidized
- Stays colorless when reduced
- Acts as an indicator
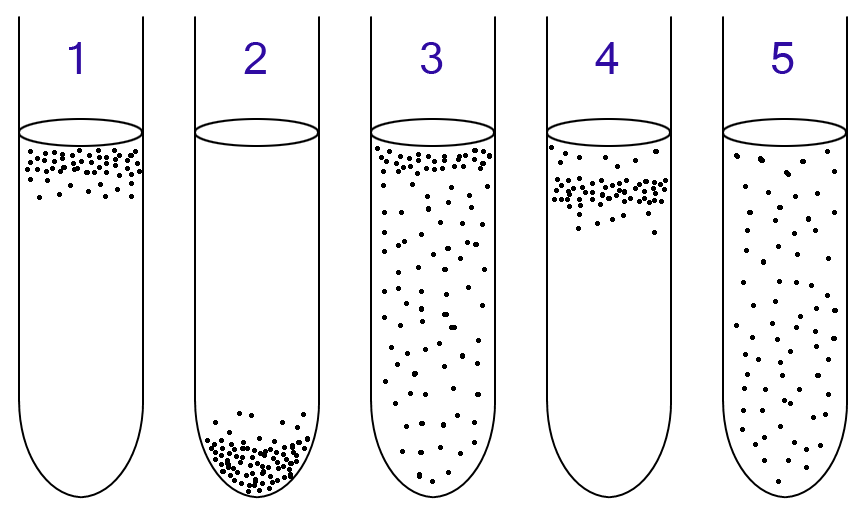
- Growth Patterns:
- Aerobic zone (pink at the top, oxidized area)
- Anaerobic at the bottom
- Aerotolerant (even turbidity throughout the entire tube)
- Facultative anaerobe (growth at the top and straight down the middle to the bottom)
- Strict anaerobe (pink at the top, growth straight down to the bottom, purple at the bottom)
- Strict aerobe (Pellicle at the top; purple growth straight down towards the bottom and is purple)
- Microaerophile (pink at the top and purple growth straight down towards the bottom)
GN Broth:
- Used to cultivate enteric bacteria
- Plated to Hektoen agar the next day after 18-24 hours
LIM Broth:
- Used to cultivate Group B streptococci (S. agalactiae)
- Plated to ChromAgar and BAP 18-24 hours later)
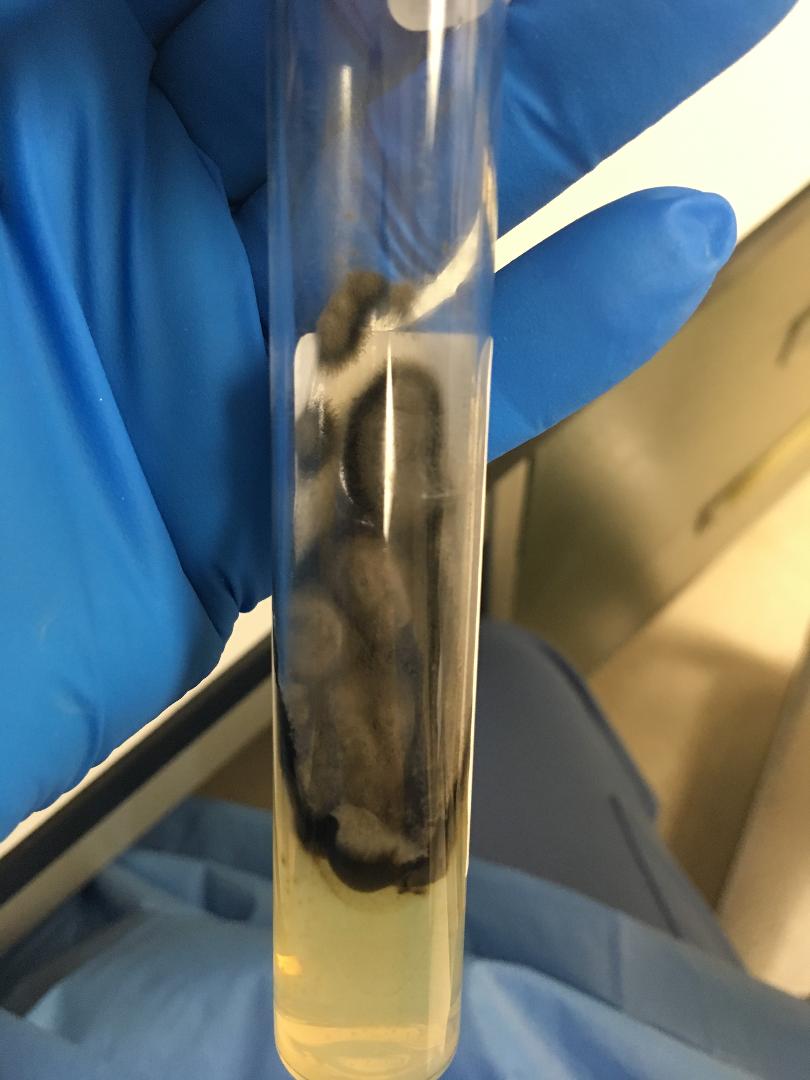
In Tubed Solid Media:
- Agar Deep Stabs
- Trypticase Soy Agar base
- Enriched with yeast extract
- Promotes growth of many organisms
- Inoculated with an inoculating needle (stab directly in the middle to about 1/4" from the bottom) and avoid getting O2 into the agar
- You can see if an organism is motile or nonmotile (turbid from the point of the stab
Aerotolerance:
Aerotolerance is the bacteria's preference to live with or without oxygen, or whether or not it can tolerate it.
- Aerobic-require oxygen
- Obligate or strict aerobes-must have oxygen for respiration and grow where oxygen is most prevalent (in broth, this is near the top)
- Facultative anaerobes-grow with or without oxygen (they can go either way)
- Oxygen is available: respire aerobically
- Oxygen is not available: respire anaerobically or ferment or reduce sulfur or nitrate instead
- Growth throughout the broth
- More growth at the top of the broth
- Anaerobic-are poisoned and killed by oxygen
- Grow only at the bottom of the broth where there is no oxygen
- Must be put in jars, anaerobic containers or anaerobic cabinets or bags with a sachet indicator
- Aerotolerant-simply tolerate oxygen but do not prefer it
- Growth will be uniform throughout the broth
- Ferment whether or not oxygen is available
- Microaerophiles-require lower levels of oxygen, but will not survive without at least some oxygen
- Grow in the middle to upper half of the broth
- Capnophiles-survive only if they have some carbon dioxide (CO2)